Empyema is a serious condition that can cause chest pain, breathlessness, and fatigue. Maria clutched her chest as another wave of pain shot through her ribs. What had started as a simple cold three weeks ago had transformed into something far more sinister. Her GP had initially prescribed antibiotics, but now, sitting in the chest physician’s office, she was hearing words that made her heart race: “empyema,” “surgical intervention,” “thoracic surgery,” and “empyema treatment.”
Empyema, a severe chest infection characterised by the accumulation of infected fluid in the pleural space surrounding the lungs, affects approximately 65,000 individuals annually.
What makes empyema particularly challenging is its progressive nature. Unlike simple pneumonia that primarily affects lung tissue, empyema involves the pleural cavity—the delicate space that allows our lungs to expand and contract with each breath. When infection invades this space, it can create thick, infected fluid collections (we call them effusions) that compress the lung, making breathing increasingly complex and potentially life-threatening.
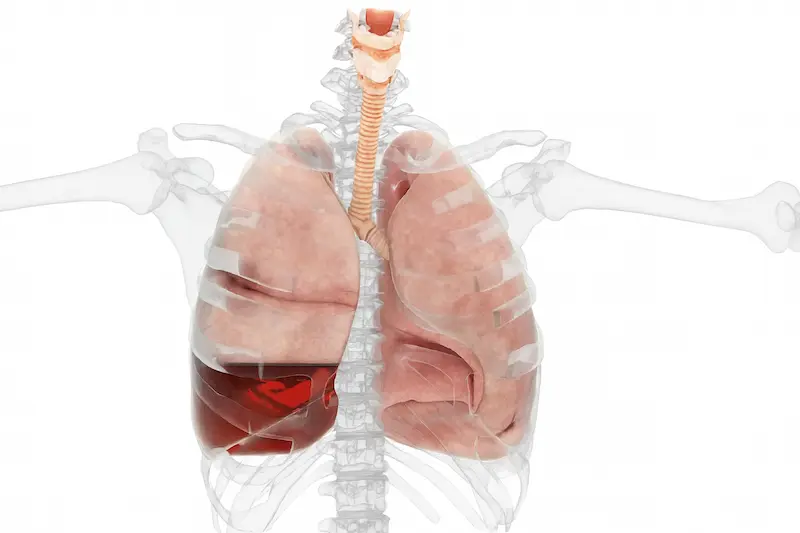
In the earliest stage, thin, infected fluid begins accumulating in the pleural space. At this point, minimally invasive procedures such as thoracentesis or chest tube drainage may effectively resolve the infection, along with long-term antibiotic therapy. Patients often experience chest pain, fever, and shortness of breath, but the condition remains highly treatable with prompt medical intervention.
As the infection progresses, the pleural fluid becomes thick and fibrous, containing white blood cells, bacteria, and cellular debris. A simple chest drain becomes less effective as the infected material thickens to the consistency of thick honey. This stage typically occurs 7-21 days after initial infection and often requires more sophisticated surgical drainage procedures or intrapleural fibrinolytic therapy. Doctors inject fibrinolytic agents into the infected pleural space, where they act as solvents to dissolve the thick material inside the chest that forms the pleural empyema. Physicians call that drug tissue plasminogen activator (TPA for short), or they also use intrapleural streptokinase.
The most advanced stage involves the formation of a pleural thickening and fibrous tissue, or a “peel” or cortex, around the lung. This rigid shell can permanently restrict lung expansion, leading to chronic breathing problems and reduced quality of life. Advanced thoracic surgery is necessary to remove this constraining layer and restore normal lung function and thoracic cavity movement. Surgery is usually reserved when intrapleural fibrinolytic therapy fails with ongoing sepsis and persistent thoracic empyema, which is when a chronic empyema develops.
When antibiotics and simple chest tube drainage fail to resolve the infection, doctors must consider surgical options. Studies show that delayed surgical intervention can lead to prolonged hospital stays, increased complications, and higher healthcare costs.
Advanced imaging techniques, such as CT scans, may reveal multiple, loculated (compartmentalised) fluid collections that doctors cannot adequately drain through simple tube placement in complex empyema thoracis. These complex collections require surgical access to ensure complete evacuation.
When the infected fluid collection compresses more than 30% of the lung volume, breathing becomes severely compromised. Doctors may require emergency surgical drainage to prevent respiratory failure.
Patients showing signs of systemic infection and sepsis, including high fever, elevated white blood cell count, and organ dysfunction, may require urgent surgical intervention to control the source of infection.
VATS has become an essential advancement in thoracic surgery, offering patients a minimally invasive alternative to traditional open surgery. This technique uses small incisions (typically 1-2 centimetres) and a tiny camera to guide surgical instruments within the chest cavity. Especially useful for patients with loculated empyema.
Benefits of VATS include:
Mr Marco Scarci is a thoracic surgeon who has performed over 500 of those VATS procedures and is the first author of the European guidelines for the treatment of empyema.
The VATS procedure typically involves:
For advanced Stage 3 empyema or cases with significant complications, such as in tuberculous empyema, open thoracotomy may be necessary. While more invasive than VATS, this approach provides surgeons with complete access to the pleural cavity, allowing for comprehensive treatment of complex infections.
Decortication procedures through open thoracotomy involve:
Robotic surgery is increasingly being utilised for complex empyema cases, combining the precision of robotic technology with the benefits of minimally invasive techniques. This approach offers enhanced visualisation and improved dexterity for intricate surgical manoeuvres.
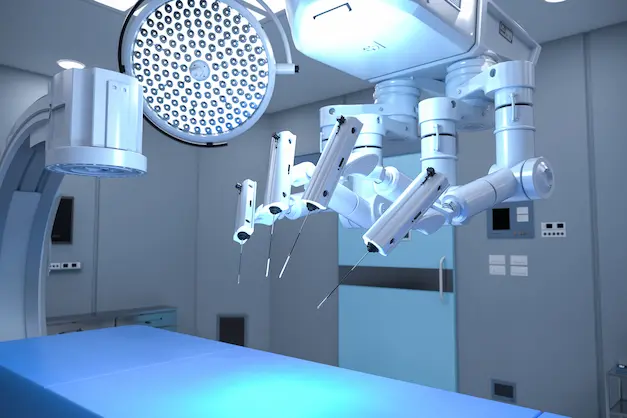
Understanding the surgical process helps patients and families prepare for the journey ahead. Experienced medical teams guide patients through each step, ensuring comprehensive care and support.
Comprehensive preoperative evaluation includes:
Sarah, who underwent VATS for Stage 2 empyema, describes her experience: "The medical team explained everything beforehand, which really helped with my anxiety. When I woke up after surgery, I could already breathe easier. The chest tube was uncomfortable, but knowing it was helping drain the infection made it bearable."
Comprehensive pain management protocols ensure patient comfort during recovery:
During the initial weeks following surgery, patients focus on:
As healing progresses, patients typically experience:
Thomas, now two years post-surgery, reflects on his journey: "I never thought I'd be grateful for something as simple as taking a deep breath. The surgery gave me my life back. I'm hiking again, playing with my grandchildren, and sleeping through the night without coughing."
Air leaks occur in 15-20% of patients but typically resolve within a few days with chest tube management. Bleeding requiring intervention is rare (less than 2% of cases) but necessitates immediate medical attention. Infection recurrence affects approximately 5-10% of patients, particularly those with underlying health conditions or compromised immune systems.
Pulmonary function recovery varies among patients, with most experiencing significant improvement within 3 to 6 months. Physical rehabilitation plays a crucial role in optimising outcomes, with structured pulmonary rehabilitation programs showing excellent results.
Dr Lisa Wang, a pulmonary rehabilitation specialist, notes:
“Patients who actively participate in breathing exercises and gradual activity progression often exceed their pre-illness functional capacity. The human body’s ability to heal and adapt is remarkable when given the proper support.”
Selecting experienced healthcare providers has a significant impact on treatment outcomes. Patients should seek medical centres with:
Experienced thoracic surgery programs typically demonstrate:

Insurance coverage for empyema surgery varies depending on the specific procedure and insurance plan. Most insurance providers, including Medicare and Medicaid, recognise surgical treatment of empyema as medically necessary when conservative treatment has failed.
Surgical treatment costs can vary significantly based on:
While doctors cannot prevent all cases of empyema, understanding risk factors and maintaining good health practices can reduce the likelihood of developing this serious condition.
Preventive measures include:
Emerging therapies continue to improve outcomes for empyema patients:
If you or a loved one is facing a diagnosis of empyema, remember that timely surgical intervention can dramatically improve outcomes and quality of life. Consulting with experienced thoracic surgeons and understanding all available treatment options empowers patients to make informed decisions about their care.
Leading medical centres offer comprehensive consultations where patients can:
Recovering from empyema takes time, but with the proper treatment and support, most patients regain normal breathing and strength.
In the battle against severe chest infection, patients are not alone. Dedicated healthcare teams stand ready to provide the expertise, technology, and support necessary to guide each person through their unique healing journey, from diagnosis to full recovery and beyond.
Contact me today to schedule your consultation. Your journey to better health starts with a single phone call.
Take the first step towards expert thoracic care. Dr. Scarci's minimally invasive surgical techniques offer the best chance for successful outcomes with faster recovery times.
London, UK
Multiple clinic locations available
24/7 emergency support available
Book your consultation through the
portal for a direct call with the surgeon