If you or a loved one has been diagnosed with a chest wall deformity, you’re not alone.
Millions of people worldwide live with conditions like pectus excavatum (sunken chest) or pectus carinatum (protruding chest), and modern medicine offers more treatment options than ever before.
This comprehensive guide will walk you through everything you need to know about chest wall deformities, from understanding your diagnosis to exploring both surgical and non-surgical treatment options that can help you feel confident and comfortable in your own body.
Chest wall deformities are structural abnormalities of the chest that can affect both appearance and function. These conditions occur when the costal cartilage connecting the ribs to the breastbone (sternum) grows abnormally, resulting in an unusual chest shape. While many people think of these as purely cosmetic concerns, chest wall deformities can sometimes affect breathing, heart function, and overall quality of life.
The most common types of chest wall deformities include:
Pectus Excavatum
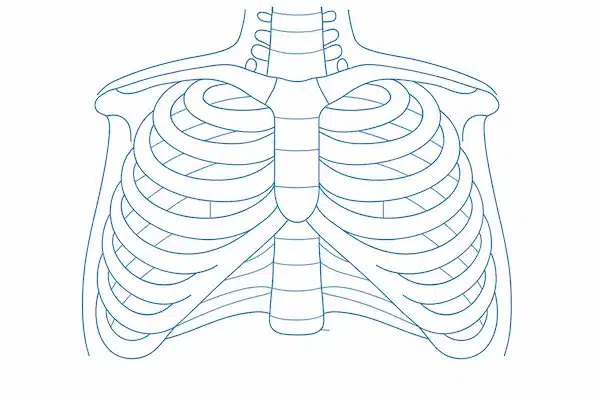
which creates a sunken or caved-in appearance of the chest
Pectus Carinatum
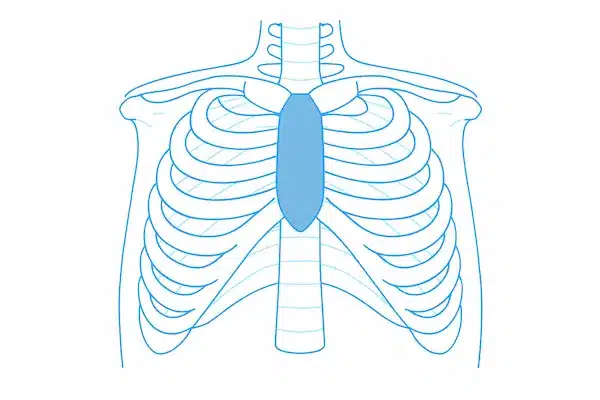
where the chest protrudes outward
Less common conditions include:
Pectus Arcuatum
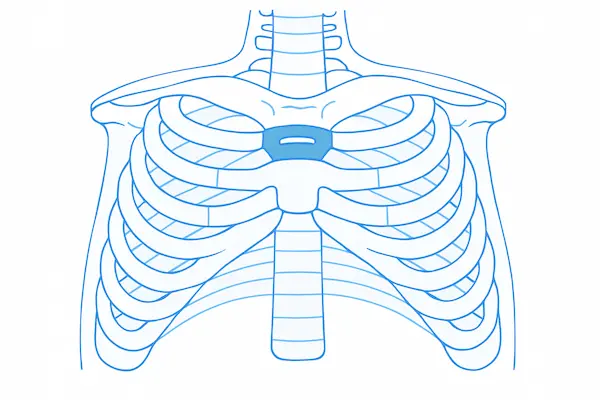
Poland syndrome, Jeune syndrome, and traumatic deformities like flail ribs.
What makes chest wall deformities particularly challenging is their visibility. Unlike many medical conditions that remain hidden, chest wall deformities can affect how you feel about your appearance, potentially impacting self-esteem, social interactions, and participation in activities like swimming or sports.
Chest wall deformities are often associated with scoliosis and connective tissue disorders, such as Marfan syndrome. They become particularly evident and can progress significantly during puberty.
Pectus excavatum, sometimes also called “funnel chest” or “sunken chest,” is the most common chest wall deformity, affecting approximately 1 in 300-400 births. This condition occurs when the sternum and several ribs grow abnormally, creating a depression in the centre of the chest. The severity can range from a mild indentation that’s barely noticeable to a deep depression that can affect heart and lung function.
Living with pectus excavatum can be challenging, especially during adolescence, when body image concerns heighten.
These feelings are entirely valid, and it’s important to know that help is available.
The impact of pectus excavatum extends beyond appearance.
For mild cases of pectus excavatum, non-surgical treatments can be effective, especially in children. The vacuum bell therapy has gained popularity as a non-invasive treatment option. This device creates suction over the depressed area, gradually pulling the sternum forward. Patients typically use the vacuum bell for 30 minutes to several hours daily, and doctors can see improvements within months of consistent use.
When non-surgical treatments aren’t sufficient, or the deformity is severe, surgical repair offers definitive treatment.
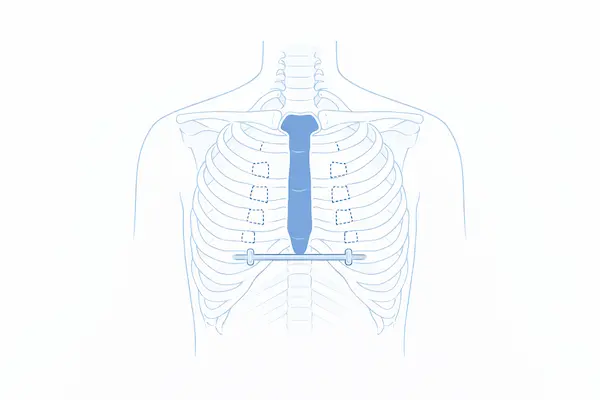
The Nuss procedure, a minimally invasive repair of pectus excavatum (MIRPE), has revolutionised treatment since its introduction.
This procedure involves inserting one or more curved metal bars beneath the sternum through small incisions on the sides of the chest. The bars push the sternum forward into a normal position and remain in place for 2-3 years while the chest wall remodels.
The Nuss procedure typically takes 1-2 hours, and most patients stay in the hospital for 3-5 days. Recovery involves managing pain, which can be significant initially but improves over the weeks.
Most patients return to light activities within 4-6 weeks and complete activities, including sports, within 3 months. The success rate is excellent, with over 95% of patients achieving good to excellent cosmetic results.
The Ravitch procedure, an older but still valuable technique, involves removing the abnormal cartilage and repositioning the sternum.
This open surgery requires a larger incision across the chest but may be preferred for certain patients, particularly adults with rigid chest walls or those with asymmetric deformities.
Some surgeons use a modified Ravitch technique that incorporates a support bar similar to the Nuss procedure.
The right approach depends on your individual anatomy and goals.
Pectus carinatum, commonly known as “pigeon chest,” occurs when the chest wall protrudes outward, creating an abnormality. This condition affects about 1 in 1,500 people and is more common in males. Unlike pectus excavatum, pectus carinatum rarely causes functional problems with the heart or lungs. Still, the cosmetic impact can be significant, particularly during the teenage years when peer acceptance feels crucial.
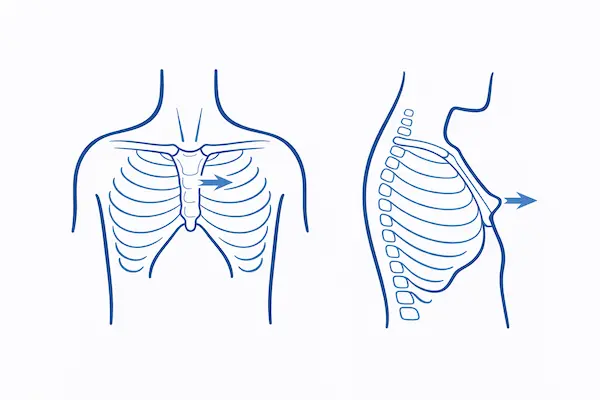
The protrusion in pectus carinatum can be symmetric, affecting the centre of the chest equally
Asymmetric, where one side protrudes more than the other
Some patients have a mixed deformity with both excavatum and carinatum components
The condition often becomes more noticeable during growth spurts in adolescence, which is also when many patients first seek treatment.
Understanding that pectus carinatum is not your fault is essential. This condition results from abnormal growth of the costal cartilages, not from anything you did or didn’t do. Many successful people, including athletes and celebrities, have lived with pectus carinatum, though modern treatment options mean you don’t have to accept the condition if it bothers you.
Chest wall bracing has emerged as a highly effective non-surgical treatment for pectus carinatum, particularly in children and adolescents whose chest walls are still flexible. Custom-made compression braces apply controlled pressure to the protruding area, gradually reshaping the chest wall over time.
Studies show excellent results when patients closely follow the treatment plan.
The bracing protocol typically involves wearing the device for 14-23 hours daily, though newer dynamic compression systems may require less wear time.
Initial measurements and fittings ensure the brace applies appropriate pressure without causing discomfort or skin problems.
Regular follow-up appointments allow for adjustments as the chest shape improves.
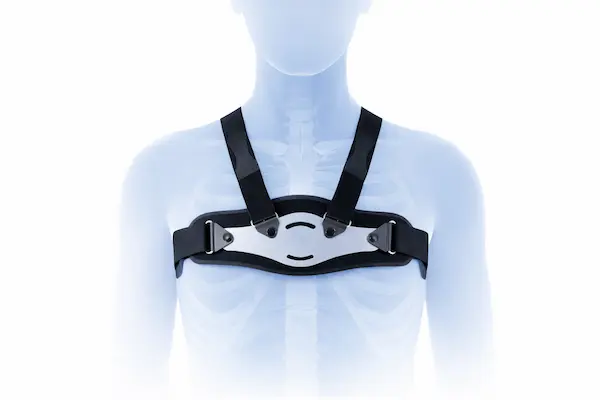
Wearing the device for 14-23 hours daily
Regular adjustments
Noticeable improvement within 3–6 months
With full correction often achieved within 12-24 months
Wear discreetly under clothing
Maintain normal activities
Participate in school
Most can do sports
Some patients initially feel self-conscious about wearing a brace, but most quickly adapt and appreciate avoiding surgery. The key to success is compliance – wearing the brace as prescribed even when improvements make it tempting to stop early.
While bracing successfully treats most pectus carinatum cases, surgery remains an option for patients with severe deformities, those who don’t respond to bracing, or adults whose chest walls are too rigid for conservative treatment. The modified Ravitch procedure is the most common surgical approach, involving the removal of the abnormal cartilage and repositioning of the sternum.
The surgical procedure typically takes 2-4 hours and requires a hospital stay of 3-5 days. Surgeons make an incision across the chest, remove the deformed cartilage segments, and may place a small bar behind the sternum for support during healing. Recovery involves managing postoperative pain and gradually returning to normal activities over 6-12 weeks. Most patients achieve excellent cosmetic results and report high satisfaction.
Surgery is rarely needed but highly effective when indicated.
Pectus arcuatum, also called currarino-silverman syndrome or pouter pigeon breast, is a rare congenital chest wall deformity characterised by protrusion of the upper sternum and adjacent cartilages. This condition creates a distinctive appearance in which the upper chest bows outward, while the lower portion may appear normal or even slightly depressed. Though less common than pectus excavatum or carinatum, this condition can be equally distressing for affected individuals. Mixed or complex chest wall deformities combine features of different conditions, such as excavatum on one side and carinatum on the other, or varying degrees of asymmetry. These complex cases require careful evaluation and often benefit from customised chest wall reconstruction. Advanced imaging techniques, such as 3D CT scanning, help surgeons plan precise corrections for these challenging deformities.
Pectus arcuatum, also called currarino-silverman syndrome or pouter pigeon breast, is a rare congenital chest wall deformity characterised by protrusion of the upper sternum and adjacent cartilages. This condition creates a distinctive appearance in which the upper chest bows outward, while the lower portion may appear normal or even slightly depressed. Though less common than pectus excavatum or carinatum, this condition can be equally distressing for affected individuals. Mixed or complex chest wall deformities combine features of different conditions, such as excavatum on one side and carinatum on the other, or varying degrees of asymmetry.
These complex cases require careful evaluation and often benefit from customised chest wall reconstruction. Advanced imaging techniques, such as 3D CT scanning, help surgeons plan precise corrections for these challenging deformities.
Treatment for pectus arcuatum and mixed chest deformity often requires a combination approach. Younger patients might start with bracing or vacuum therapy to address the prominent areas while using exercises to strengthen surrounding muscles. When surgery is necessary, surgeons tailor procedures to address each component of the deformity, sometimes requiring innovative techniques or combinations of established methods.
Insurance coverage for the treatment of chest wall deformity has become rather challenging. Some insurance plans MIGHT cover treatment when there’s documented cardiopulmonary impairment, with specific criteria varying by insurer. Common covered indications include a Haller index greater than 3.25 for pectus excavatum, documented cardiac compression, reduced pulmonary function, or exercise intolerance.
The insurance approval process typically requires comprehensive documentation, including physical examination findings, imaging studies (CT or MRI), pulmonary function tests, and sometimes cardiac evaluation.
Some patients can present with congenital heart disease, especially mitral valve prolapse, and connective tissue disorder.
The emotional impact of living with a chest wall deformity often equals or exceeds the physical challenges. Many patients experience anxiety, depression, social withdrawal, or body dysmorphic concerns related to their condition. These feelings are entirely normal and valid – your emotional well-being is just as important as your physical health.
The emotional impact of living with a chest wall deformity often equals or exceeds the physical challenges. Many patients experience anxiety, depression, social withdrawal, or body dysmorphic concerns related to their condition. These feelings are entirely normal and valid – your emotional well-being is just as important as your physical health.
Adolescents and young adults may face particular challenges as they navigate dating, sports participation, and social situations that involve removing their shirt. The fear of judgment or questions about their appearance can lead to avoidance behaviours that limit life experiences. Professional counselling can provide valuable coping strategies and help build confidence, whether or not you choose treatment.
Support groups, both in-person and online, connect you with others who understand your experience firsthand. These communities offer practical advice, emotional support, and inspiration from those who’ve successfully navigated treatment. Many patients find that sharing their story and helping others reduces their own anxiety and builds resilience.
Family support plays a crucial role in treatment success, particularly for younger patients. Parents should maintain open communication, validate their child’s concerns without minimising them, and involve them appropriately in treatment decisions. Siblings may also need support in understanding the condition and the treatment process. Family therapy can help navigate the challenges posed by chest wall deformities to the entire family system.
Recovery from chest wall deformity treatment, whether surgical or non-surgical, requires patience, dedication, and proper support. The recovery timeline varies depending on the treatment type, your age, and overall health. Understanding what to expect helps you prepare mentally and practically for the journey ahead.
Immediate postoperative period: pain management, prevention of complications (nerve blocks, epidural catheters, multimodal analgesia).
Walking within 24 hours, discharged home in 3–5 days.
First two weeks at home: rest and assistance with daily activities.
Physical therapy: starts with breathing exercises and gentle range-of-motion.
Later therapy: posture training, core strengthening, gradual return to normal activities.
Return to school/work: 3–4 weeks; resume sports after 3 months (contact sports may be restricted longer).

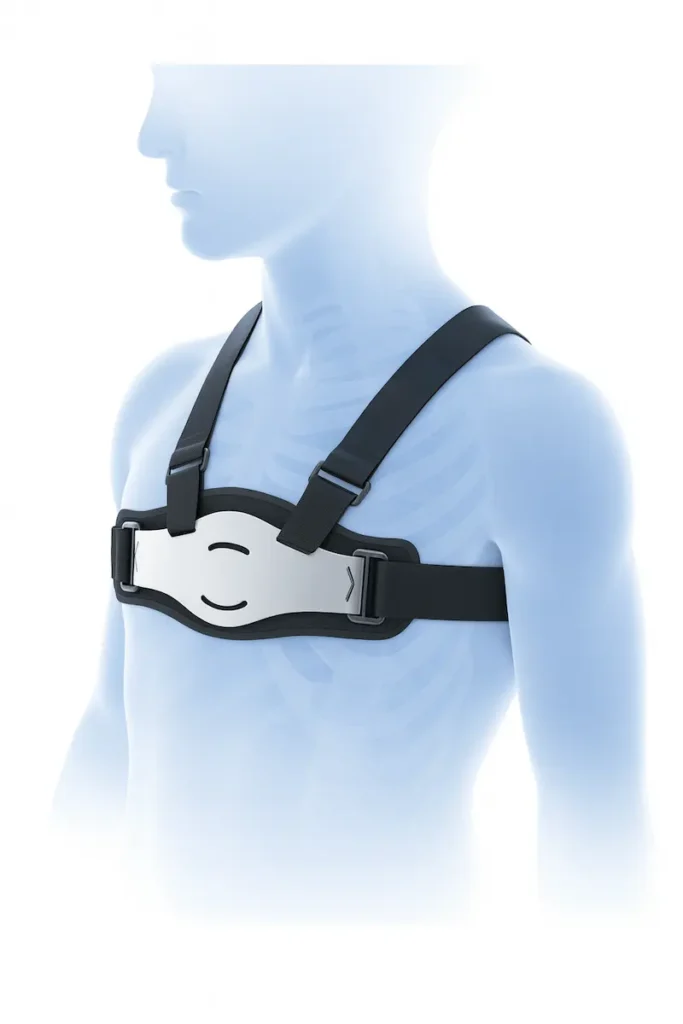
Non-surgical treatments like bracing or vacuum bell therapy require their own form of dedication. Success depends on consistent use and regular follow-up appointments for adjustments. Many patients find it helpful to establish routines that incorporate treatment into daily life, such as wearing the vacuum bell while studying or watching TV. Keeping a treatment diary can help track progress and maintain motivation throughout treatment.
Deciding when to seek treatment for a chest wall deformity is highly personal and depends on various factors, including severity, symptoms, age, and quality of life impact. There’s no universal “right time” – what matters is finding the approach that aligns with your needs and goals.
For children and adolescents, timing considerations include skeletal maturity, psychological readiness, and the potential for non-surgical interventions. Early intervention with bracing for pectus carinatum often yields better results than waiting until skeletal maturity. However, surgeons usually delay surgical correction of pectus excavatum until the adolescent growth spurt is nearly complete to reduce the risk of recurrence.
Adults seeking treatment should consider their lifestyle, career demands, and support system when planning intervention. While the chest wall becomes less flexible with age, making some treatments more challenging, many adults successfully undergo correction with excellent results. The decision often comes down to whether the physical or psychological impact of the deformity outweighs the temporary disruption caused by the treatment.
For children and adolescents, timing considerations include skeletal maturity, psychological readiness, and the potential for non-surgical interventions. Early intervention with bracing for pectus carinatum often yields better results than waiting until skeletal maturity. However, surgeons usually delay surgical correction of pectus excavatum until the adolescent growth spurt is nearly complete to reduce the risk of recurrence.
Take time to thoroughly research your options, connect with experienced medical teams, and consider all aspects of treatment, including physical, emotional, and financial factors. Don’t let fear or embarrassment prevent you from seeking help – medical professionals who specialise in chest wall deformities understand the impact these conditions have. They are committed to helping you achieve the best possible outcome.

Expert answers to common questions about thoracic surgery, recovery and what to expect.
There are different types of congenital chest wall deformities. The most common is the pectus excavatum, also called, in simpler terms, funnel chest. In this condition, the anterior portion of the chest sinks in and forms like a funnel. There are different variants based on the severity of the deformity (mild, moderate, or severe) and its shape. Some involve only the bottom part of the chest, others the entire breastbone. Sometimes the defect is wide and long, and it is called the Grand Canyon variant. This deformity affects nearly 2/3 of all patients and is more prevalent in males. Another common variant is the pectus carinatum, also called pigeon chest. In this condition, the breastbone sticks forward like the bow of a ship. It also has different grades of severity, and sometimes it can also be visible under clothes. This condition affects about 1/3 of the remaining cases. Lastly, there is a rare variant called pectus arcuatum, which combines the two previously mentioned defects. Very often this is wrongly diagnosed as pectus excavatum as the chest does sink in, but, more importantly, it also sticks out. Doctors need to be familiar with this condition and properly diagnose it, as an incorrect diagnosis can lead to the wrong treatment.
Symptoms vary widely depending on the type and severity of the defect. Some patients with mild conditions have no physical symptoms or are only very mildly symptomatic. Others with severe defects may experience shortness of breath and anterior rib cage pain, especially after exercise. This pain is relatively non-specific, and it is mainly related to an asymmetry in the rib cage that responds differently to mechanical stress. Shortness of breath is also relatively common, but unfortunately, it is difficult to diagnose, as most patients are young and fit at rest. The problems only become evident during sub-maximal exercise. In this patient group, a cardiopulmonary exercise test might be the best approach to document symptoms. Static lung function is not helpful in this scenario, nor is a standard chest X-ray.
Marco Scarci is renowned for his expertise in thoracic surgery and lung cancer care. Patients consistently highlight his compassionate approach, clear communication, and exceptional skill in delivering personalised treatment plans. Many praise his ability to put them at ease during challenging times and commend the successful outcomes of their surgeries. His dedication to patient care and cutting-edge techniques has earned him glowing reviews and deep gratitude from those he's helped.
Contact me today to schedule your consultation. Your journey to better health starts with a single phone call.
Take the first step towards expert thoracic care. Dr. Scarci's minimally invasive surgical techniques offer the best chance for successful outcomes with faster recovery times.
London, UK
Multiple clinic locations available
24/7 emergency support available
Book your consultation through the
portal for a direct call with the surgeon