Facing a lung cancer diagnosis is challenging enough without the added uncertainty of understanding treatment costs. Whether you’re exploring private options to avoid NHS waiting times or you’re an international patient seeking specialist care in the UK, knowing what to expect financially helps you plan with confidence. This guide breaks down the real costs of lung cancer surgery in the UK for 2025–2026, explains what affects pricing, and offers practical advice for navigating your options.
Lung cancer care represents a significant financial burden on the UK economy, with the costs of diagnosis and treatment contributing substantially to national healthcare expenditure. Private healthcare can provide a team approach to lung cancer treatment, involving multiple specialists.
Before diving into the detail, here are the concrete figures most patients want to know. These are self-pay price ranges for private lung cancer surgery in the UK, based on current 2025–2026 pricing at major centres. Patients can access second opinions and virtual consultations through private healthcare for lung cancer.
Typical private lung cancer surgery costs:
- VATS wedge resection: roughly £12,000–£18,000 in major UK centres
- VATS lobectomy: typically £18,000–£28,000 (often highest in central London)
- Open lobectomy or pneumonectomy: often £22,000–£35,000 depending on complexity and length of stay
The average cost of lung cancer treatment in the United Kingdom is estimated to be between £4,000 and £19,500, with the mean cost of radiotherapy for lung cancer around £2,655. Surgery and systemic anti-cancer therapy (SACT) are generally the most expensive treatments for lung cancer. A study found that patients diagnosed with lung cancer at earlier stages generally incur lower treatment costs compared to those diagnosed at later stages. Compared to lung cancer, prostate cancer treatment costs in the UK can differ significantly, with variations in expenditure depending on treatment modality (such as systemic anti-cancer therapy, radiotherapy, or resection) and stage at diagnosis, reflecting different treatment patterns and overall costs.
These figures usually include surgeon and anaesthetist fees, hospital charges, theatre time, and a standard post-operative hospital stay. However, they typically do not cover pre-operative diagnostics (such as PET-CT scans or lung function tests) or ongoing oncology treatment like chemotherapy or radiotherapy.
For NHS patients, lung cancer surgery is free at the point of use for eligible UK residents. That said, waiting times, cancer stage, and whether the tumour is operable often influence whether cancer patients consider private healthcare for faster access to treatment.
The rest of this article will break down exactly what affects cost, how to budget effectively, and how Mr Marco Scarci’s team in London structures pricing and quotes for self pay and insured patients alike.
What affects the cost of lung cancer surgery in the UK?
Lung cancer surgery costs vary significantly between a straightforward keyhole lobectomy and a complex open procedure requiring intensive care. London prices tend to sit at the upper end compared with regional providers across England, Scotland, and Wales. Surgery may be recommended to remove tumors, lymph nodes, or even an entire lung in cases of primary lung cancer, and choosing private thoracic surgery in London can influence both cost and access. Initial consultations for private lung cancer treatment often range from £250 to £350.
Main cost drivers include:
- Type of operation: wedge resection, segmentectomy, lobectomy, bilobectomy, pneumonectomy, or chest wall resection all carry different complexity levels and pricing
- Surgical approach: video-assisted thoracoscopic surgery (VATS), robotic-assisted procedures, or traditional open thoracotomy affect theatre time, recovery, and overall cost. Minimally invasive techniques like Video-Assisted Thoracoscopic Surgery (VATS) or robotic-assisted surgery are generally more expensive due to equipment costs. Robotic-assisted thoracic surgery is a minimally invasive option that can enhance precision in lung cancer surgery.
- Hospital location: central London private hospitals typically charge 10–20% more than regional providers because of the level of care they afford to patients, those are like NHS hospitals in terms of safety and patients’ support. Hospitals in the London area, especially in Harley Street, can be 25–35% more expensive than the national average for lung cancer surgery.
- Length of hospital stay: an uncomplicated VATS lobectomy may require only 2–3 nights, while open procedures or those with complications can extend to 5–10 days or more
- Need for HDU or ICU care: high-dependency or intensive care unit stays add substantial daily charges
- Consultant fees: very experienced or subspecialist thoracic surgeons may charge higher fees reflecting their expertise
- Additional procedures: mediastinal lymph node dissection, pleural procedures, or reconstruction work add to the final bill
Package prices quoted online are usually “guide prices.” A personalised treatment cost is confirmed after your initial consultation and review of your CT scan, PET-CT, and lung function results.
Breakdown of private lung cancer surgery costs
Self pay patients are often quoted a single “fixed price” for lung cancer surgery. Understanding what this typically includes—and what it doesn’t—helps you compare quotes and avoid unexpected charges, and an honest guide to the real cost of private cancer treatment in the UK can further clarify what to expect at each stage.
Initial consultation
- Initial consultation with a thoracic surgeon: usually £250–£350 in London (face-to-face or virtual), often excluding diagnostic imaging
Pre-operative diagnostics
- CT scan: £400–£900
- PET-CT: £1,000–£1,800
- Lung function tests: £150–£300
- Bronchoscopy or EBUS (when needed): £1,500–£3,000
Surgeon’s fee
- Surgeon’s fee: commonly £8,000–£15,000 for a lobectomy in private practice, depending on complexity and resection type
Anaesthetist’s fee
- Anaesthetist’s fee: typically £1,200–£2,500 for major thoracic surgery
Hospital and theatre charges
- Hospital and theatre charges: the largest portion of the bill, often £10,000–£20,000 for a 3–5 day stay including theatre time, ward or HDU bed, routine blood tests, and medications
Intensive Care Unit surcharge
- Intensive Care Unit surcharge: a planned or unplanned ICU stay (e.g. 1–2 nights) can add £2,000–£5,000+ per night in some London hospitals
Early follow up and routine post-operative imaging
- Early follow up and routine post-operative imaging: follow-up consultation £200–£350, chest X-ray or CT £150–£700
A typical “all-inclusive” quote for a standard VATS lobectomy surgery in a London clinic in 2025–2026 might therefore sit between £18,000 and £28,000 depending on these factors.
Oncology treatments such as chemotherapy, immunotherapy, or targeted therapies are usually costed separately and not bundled into the surgical package. The same applies to curative radiotherapy if required.
Comparing NHS and private lung cancer surgery in the UK
The National Health Service provides lung cancer treatment free at the point of use for UK residents, funded through general taxation. Private treatment offers fast access, faster scheduling, and more flexibility but comes with direct healthcare costs.
Key comparison points:
| Aspect | NHS | Private |
|---|---|---|
| Direct cost to patient | Free for UK residents | Self pay or via health insurance |
| Waiting times | Can average 62 days from referral to treatment | Often 1–2 weeks from consultation to surgery |
| Choice of surgeon | Assigned based on availability | Patient chooses their consultant |
| Hospital environment | Standard NHS ward | Often single rooms with additional amenities |
| Indirect costs | Time off work, travel, waiting anxiety | Treatment cost plus travel/accommodation |
| Early stage lung cancer often benefits from prompt surgery. Some patients consider private lung cancer treatment to avoid delays when local NHS waiting times exceed several weeks. This can be particularly important when lung cancer screening has identified a suspicious lung tumour requiring rapid diagnosis and intervention. | ||
| A common approach among UK patients is to receive their cancer diagnosis and oncology treatments (such as chemotherapy or radiotherapy) via the NHS while opting to have surgery privately, then returning to NHS follow up if appropriate. This blend of care can offer the speed of private surgery with the comprehensive support of NHS cancer care. | ||
| Clinical standards and multidisciplinary decision-making are similar across both settings. Many private thoracic surgeons, including Mr Marco Scarci, also hold substantive NHS consultant posts, ensuring consistent expertise regardless of where you receive treatment. |
Practical example: A patient in London with an early stage lung cancer diagnosis might wait several weeks on an NHS list for lobectomy surgery. By choosing private VATS lobectomy with Mr Scarci, that same patient could have their operation within 1 week of their consultation, potentially improving outcomes without compromising on surgical quality.
In addition to UK options, some patients look abroad for treatment. In Turkey, lung cancer treatment can save patients 50-70% compared to the UK, and Turkey is known for its medical tourism, treating thousands of international patients annually for lung cancer. Patients in Turkey can also access lung cancer treatment 2-4 times faster than in the UK, making it an attractive option for those seeking both cost savings and fast access to care, although improving lung cancer screening and early detection in the UK remains crucial for outcomes regardless of where treatment takes place.
How much does each type of lung cancer operation typically cost?
The precise treatment cost depends on the exact procedure recommended for your primary lung cancer. To understand what these procedures involve clinically, from preparation through recovery, it can help to review what to expect from lung cancer surgery and how to access expert care. Here are typical 2025–2026 price bands for major thoracic operations in private UK hospitals.
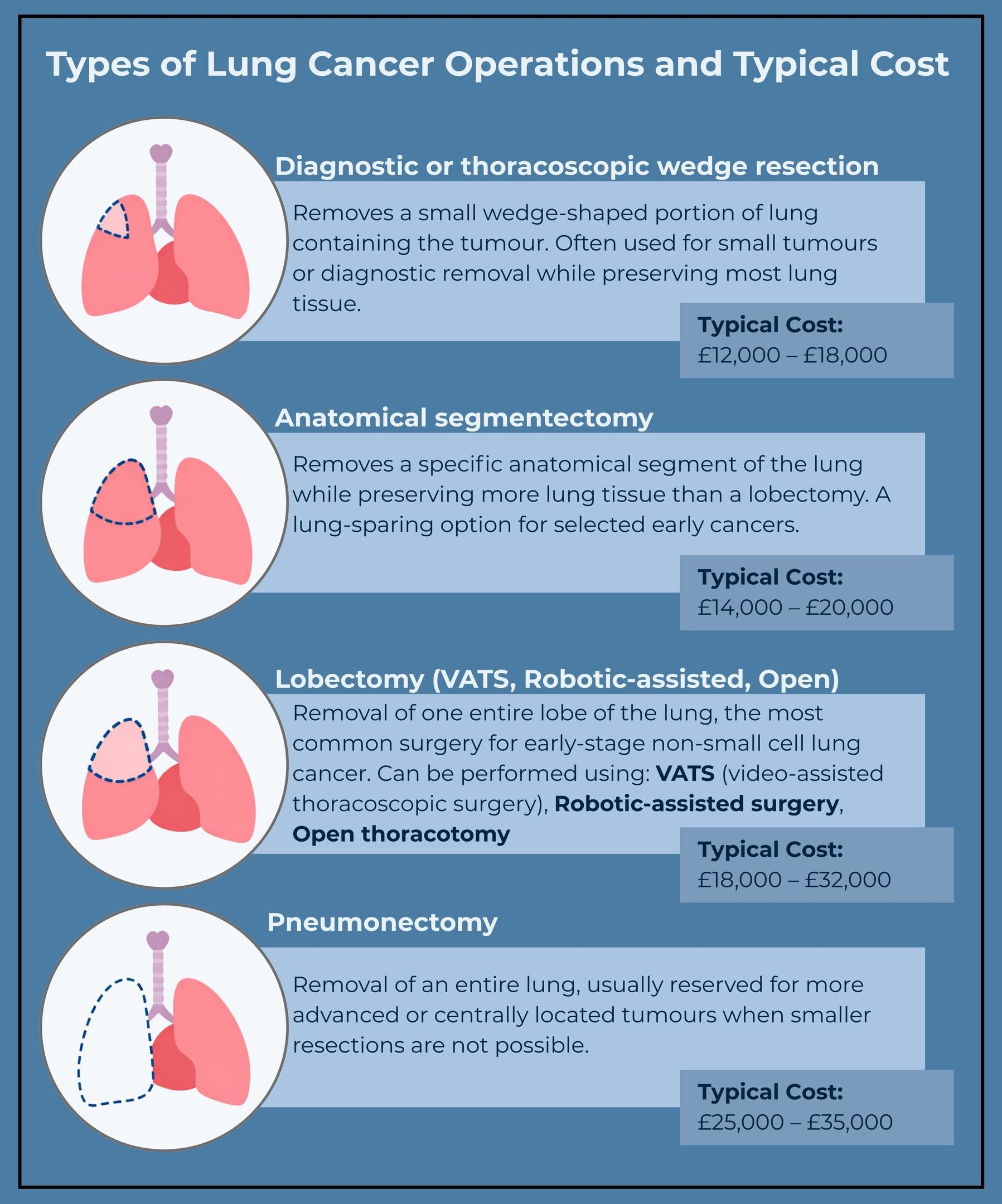
Diagnostic or thoracoscopic wedge resection
This procedure removes a small, wedge-shaped section of lung tissue and is often used for diagnostic purposes or to remove small lung tumours. Typical cost: £12,000–£18,000 depending on approach and hospital.
Anatomical segmentectomy
Minimally invasive lung-sparing surgery options include lobectomy and segmentectomy, which preserve lung function.
A lung-sparing cancer operation that removes a specific segment of the lung while preserving more tissue than a lobectomy. Generally similar or slightly higher than wedge resection: £14,000–£20,000.
VATS lobectomy
Lobectomy lung surgery involves the removal of one lobe of the lung when there is a problem in that specific area.
The most common operation for treating lung cancer at an early stage, particularly non-small cell lung cancer. Video-assisted thoracoscopic surgery removes one lobe of the lung through small incisions, and there are several useful insights on lung cancer surgery that can help patients understand risks, benefits, and recovery. Typical cost: £18,000–£28,000.
Robotic-assisted lobectomy
Robotic-assisted thoracic surgery is a minimally invasive option that can enhance precision in lung cancer surgery.
Uses robotic systems (such as the da Vinci platform) for enhanced precision in complex cases, and many patients are now considering robotic-assisted lung cancer surgery as a minimally invasive option with potential benefits in recovery and precision. This may attract a premium over standard VATS due to technology and theatre costs: £20,000–£32,000.
Open lobectomy via thoracotomy
Lobectomy lung surgery involves the removal of one lobe of the lung when there is a problem in that specific area.
When minimally invasive approaches aren’t suitable, traditional open surgery is performed through a larger incision. Often in the £20,000–£30,000 range, with price sensitive to expected pain control needs and length of stay.
Pneumonectomy
Surgery may be recommended to remove tumors, lymph nodes, or even an entire lung in cases of primary lung cancer.
Removal of an entire lung, reserved for more advanced cases where the cancer cannot be treated with a smaller resection. Usually towards the upper end of the range: £25,000–£35,000 due to longer hospital admissions and higher risk.
These figures assume an uncomplicated stay of around 3–7 nights in a private London hospital. Extended stays, re-admissions, complications, or additional procedures (such as chest wall resection) can increase the final cost. Always ask for clarification on what happens if your stay is longer than expected or if the operation needs to be converted from VATS to open.
Hospital stay and recovery after lung cancer surgery
The journey through lung cancer surgery doesn’t end in the operating theatre—your hospital stay and recovery period are just as crucial to achieving the best possible outcome. For most patients in the UK, the typical hospital stay after lung cancer surgery ranges from 5 to 10 days, depending on the type of procedure performed, your overall health, and how quickly you recover. Minimally invasive techniques, such as VATS or robotic-assisted surgery, often mean a shorter hospital admission and a smoother recovery compared to traditional open surgery.
During your hospital stay, you’ll be closely monitored by a multidisciplinary team of healthcare professionals, including thoracic surgeons, specialist nurses, physiotherapists, and pain management experts. Their goal is to support your recovery, manage pain effectively, and reduce the risk of complications such as infection, bleeding, or respiratory issues. Early mobilisation, breathing exercises, and tailored physiotherapy are all part of the standard recovery plan to help restore lung function and get you back on your feet, supported by an experienced thoracic surgery care team.
Once you’re discharged, your recovery continues at home. Most patients are advised to rest and avoid strenuous activities for several weeks, gradually increasing activity as strength returns. Pain management remains important—your consultant will prescribe appropriate medication and provide guidance on managing discomfort. A healthy diet, good hydration, and regular follow-up appointments are essential to monitor your progress and catch any early signs of complications.
It’s vital to be aware of symptoms that may indicate a problem after surgery, such as persistent pain, fever, shortness of breath, or unusual swelling. Promptly reporting these to your healthcare team can help prevent more serious issues and ensure a smooth recovery.
The cost of your hospital stay and recovery can vary significantly based on your treatment plan, the complexity of your surgery, and whether you are an NHS or private patient. For those with private medical insurance, many policies cover the hospital stay, consultant fees, and standard post-operative care, but it’s important to confirm the details with your insurer. Self pay patients should ensure their fixed-price package includes all expected recovery costs, and ask about potential additional charges if complications arise or if a longer stay is needed, particularly when choosing an expert thoracic surgeon in London for minimally invasive lung cancer surgery.
Your recovery plan may also include further cancer treatment, such as chemotherapy, targeted therapies, or radiotherapy, depending on your cancer stage and multidisciplinary team recommendations. These treatments can be delivered as an inpatient or outpatient, and their costs will depend on your chosen provider and insurance coverage.
Navigating the recovery phase can feel overwhelming, but working closely with expert consultants and your wider healthcare team ensures you have the support and information you need. Whether you’re accessing private lung cancer treatment at a leading London clinic or through the national health service, understanding your treatment options, expected recovery timeline, and associated healthcare costs will help you make informed decisions and plan ahead.
Ultimately, a successful recovery after lung cancer surgery relies on early diagnosis, expert surgical care, and a personalised treatment plan that addresses both your medical and practical needs. By staying proactive, attending all follow-up appointments, and communicating openly with your care team, you can minimise complications, manage your lung cancer treatment cost, and focus on regaining your health and quality of life.
Insurance, self-pay and finance for lung cancer surgery
Most UK patients access private lung cancer surgery either through private medical insurance or by paying directly as self pay patients. Understanding your options helps you plan effectively. Most private medical insurance policies will cover at least part of the cost of private lung cancer treatment, including diagnostic tests, surgery, chemotherapy, targeted therapies, and follow-up care. Self-funding is a common route for those without private medical insurance or who are ineligible for cancer care coverage. Many private healthcare providers in the UK offer financing options that allow patients to pay for private surgeries on a monthly basis, and dedicated guides on flexible finance options for thoracic surgery can help clarify what is available.
Private medical insurance
Most UK PMI policies from major insurers—including Bupa, AXA Health, Aviva, and Vitality—cover lung cancer surgery provided the policy is active and the condition is not excluded as pre-existing.
Key points for insured patients:
- Check with your insurer: Patients should check with their insurer and get a claim authorized before booking an appointment with a private pulmonologist if they have health or private medical insurance.
- What’s covered: Typical elements covered include consultant fees, anaesthetist’s fee, hospital stay, theatre time, and standard post-operative care
- Policy excess: Check your policy excess (the amount you pay before insurance kicks in) and any benefit limits
- Fee arrangements: Some policies have “fee-assured” or “fee-capped” arrangements—confirm whether your surgeon participates
Mr Marco Scarci’s team is experienced in working with major UK and international insurers and can assist with authorisation codes and clinical documentation to streamline the process.
Self pay
Self pay “fixed price” packages at London private hospitals typically bundle surgeon, anaesthetist, hospital, and theatre charges into one figure.
When requesting a quote, ask explicitly:
- Pre-operative imaging: Is pre-operative imaging (CT, PET-CT) included?
- Lung function tests: Are lung function tests covered?
- ICU/HDU stay: What happens if ICU/HDU stay is needed?
- Operation changes: What if the operation takes longer than expected or converts from VATS to open?
Mr Marco Scarci’s team provides clear, written quotes once imaging and lung function are reviewed, so you know exactly what to expect before committing to treatment.
Finance and staged payments
Some hospitals offer payment plans or third-party finance options for eligible patients, particularly for higher-cost procedures. Interest rates and contractual terms vary, so check these carefully. Mr Scarci’s practice does not provide financial advice, but the team can direct you to hospital finance departments for further information, including options available at centres such as Elstree Outpatients Centre.
Example pathway comparison:
- Insured patient: After receiving their lung cancer diagnosis, they contact their insurer for pre-authorisation, attend consultation with Mr Scarci, and proceed to surgery with most costs covered directly. They may pay only their policy excess.
- Self pay patient: After consultation and review of scans, they receive a written quote for the full package. Payment is made before or at the time of surgery, with clear documentation of what’s included.
How Mr Marco Scarci approaches lung cancer surgery and costs
Mr Marco Scarci is a London-based consultant thoracic surgeon specialising in minimally invasive lung cancer surgery. Working both privately and within the NHS, he brings expert consultants-level experience to every case while maintaining transparent communication about treatment costs.
What to expect from Mr Scarci’s practice:
- Consultations: Face-to-face and virtual options are available for UK and international patients with suspected or confirmed lung cancer
- Surgical approach: Focus on keyhole (VATS) and, where appropriate, robotic techniques to reduce pain, shorten hospital stay, and potentially lower costs compared with prolonged open procedures
- Individualised treatment plan: Every patient receives a plan based on their tumour stage, lung function, and overall health, discussed in a multidisciplinary setting where appropriate
- Clear pricing: Written, itemised quotes for surgery that clarify:
- Surgeon’s fee
- Anaesthetist’s fee
- Hospital/theatre package
- Expected length of stay
- Insurance support: The practice is experienced in working with major UK insurers and can assist with authorisation codes and clinical documentation
- Self pay transparency: Patients can request an estimate early in the process (after review of scans), and unexpected changes (such as need for ICU) are discussed openly wherever possible
Prospective patients can contact Mr Scarci’s office directly to discuss likely cost ranges before committing to treatment, using dedicated channels for private thoracic surgery appointments in London. The clinical decision on whether surgery is appropriate always comes before financial considerations, and many people find reassurance in reading patient testimonials about thoracic surgery care when weighing up their options.
Practical tips for patients planning for lung cancer surgery costs
Financial planning adds stress at an already difficult time. These practical steps can make navigating lung cancer costs easier and help you feel more in control.
Before your consultation
- Gather your records: Bring previous imaging reports (CT, PET-CT), biopsy results, and clinic letters. These help the surgeon define the likely operation and cost range more accurately.
- Check your insurance: Review any existing private medical insurance policy for cancer cover, exclusions, and whether you need a GP referral before seeing a specialist.
- Research your options: Look at several hospitals and surgeons, focusing on experience with minimally invasive procedures and support services.
During your consultation
- Ask specific questions: Which operation is being recommended (e.g. VATS lobectomy)? Is ICU or HDU stay anticipated?
- Request written estimates: Ask for a fixed-price quote and clarify what happens if the operation needs to convert from VATS to open, or if your stay extends beyond the expected length.
- Understand the full picture: Ask about follow up appointments, diagnostic tests you may still need, and how ongoing cancer treatment (chemotherapy, radiotherapy) will be coordinated.
When comparing hospitals
- Look beyond the headline price: Compare surgeon experience, availability of minimally invasive techniques, intensive care availability, and post-operative support.
- Factor in practical costs: Travel, accommodation for relatives, and time off work can add up, especially if you’re choosing a London clinic from outside the area.
- Consider the benefit of expertise: Specialist thoracic surgeons with high volumes of lung cancer surgery often achieve better outcomes—this may be worth the additional investment.
Coordinating with the NHS
- Ask about mixed pathways: Your surgeon can advise whether surgery can be done privately while chemotherapy or radiotherapy is delivered via the NHS, where appropriate.
- Ensure continuity of care: Make sure discharge summaries and operative reports are shared with your NHS team so your ongoing cancer care remains seamless.
- Return to NHS follow up if needed: Many patients have their surgery privately then continue surveillance and additional treatment through the NHS.
Research shows that outcomes for lung cancer surgery are strongly influenced by tumour stage at diagnosis and the experience of the surgical team. Lung cancer screening and prompt action on symptoms can lead to earlier diagnosis and better results regardless of whether you choose NHS or private treatment.
While the figures can seem daunting, many patients successfully navigate a blend of NHS and private care with proper planning and clear communication. Whether you’re dealing with societal costs like unpaid care and time off work, or simply trying to understand what your health insurance covers, taking the time to research pays off. Home-based private care for lung cancer treatment is becoming more common, allowing patients to receive care in a comfortable setting.
Mr Marco Scarci and his team understand that facing lung cancer involves both medical and practical challenges. They’re available to discuss the clinical aspects of your care alongside the logistical questions about cost, timing, and treatment options. If you’re considering lung cancer surgery in the UK, reaching out for an initial consultation is the first step toward clarity—both about your treatment plan and the investment involved.