When lung cancer requires more than a standard lobectomy, your cancer team may recommend removing an entire lung. This major surgery carries significant implications for your recovery and daily life, but with proper preparation and specialist care, many patients go on to lead active, fulfilling lives with a single lung.
Overview: what is a pneumonectomy for lung cancer?
A pneumonectomy is a major lung surgery for lung cancer where a surgeon removes one entire lung—either the right lung or left lung—to achieve complete removal of the tumour. During a pneumonectomy, the surgeon makes a cut (incision) on the side of your body and removes the affected lung. This extensive procedure is typically offered when smaller resections cannot safely clear all the cancer cells.
Most pneumonectomies are performed for non small cell lung cancer (NSCLC), particularly when the tumour is large, centrally located near the main airway, or has spread across multiple lobes of the lung. In these situations, a lobectomy or segmentectomy would leave disease behind, making pneumonectomy the best option for cure. Pneumonectomy is often used for NSCLC when tumors involve the main stem bronchus or multiple lobes.
The cancer is located in the central part of the lung or involves the main bronchus and cannot be treated with less extensive procedures like lobectomy.
Living with one lung is entirely possible. The remaining lung expands over time, and the chest cavity gradually adapts to the change. While breathlessness on exertion and a longer recovery period are expected, many people return to normal household activities, work, and even gentle exercise within several weeks to months. The key is careful patient selection and thorough preparation. After a pneumonectomy, the remaining lung can usually take in enough oxygen and remove enough carbon dioxide to provide sufficient respiratory function. The empty space in the chest fills with fluid after a pneumonectomy, and the mediastinum may shift. Most individuals can survive with one lung if it provides enough oxygen and removes enough carbon dioxide to sustain bodily needs.
In the UK, pneumonectomy is always planned and delivered by specialist thoracic surgeons working within multidisciplinary lung cancer teams. Pneumonectomy is a technically complex procedure that requires highly refined surgical expertise. This article, written from the perspective of Mr Marco Scarci, consultant thoracic surgeon in London, covers everything you need to know—from indications and preparation through to the operation itself, risks, recovery, and alternatives.
Key points:
- Pneumonectomy means surgical removal of one whole lung
- It is most commonly performed for non small cell lung cancer when lung-sparing options are not feasible
- Many patients adapt well to life with a single lung
- The procedure is performed by specialist thoracic surgery teams following MDT assessment
How a pneumonectomy fits into lung cancer treatment
Pneumonectomy sits at one end of the spectrum of lung cancer surgery options. There are three main types of lung cancer surgery: lobectomy, pneumonectomy, and wedge resection. Understanding where it fits helps you see why your cancer team might recommend this approach over others.
Lung cancer treatment options to treat lung cancer include:
- Wedge resection – Very small, peripheral tumours
- Segmentectomy – Small tumours in specific lung segments
- Lobectomy – Most common; removes one lobe
- Sleeve lobectomy – Central tumours where airway can be reconstructed
- Pneumonectomy – Large or central tumours involving multiple lobes or major structures
- Radiotherapy/SABR – Early stage disease in patients unfit for surgery
- Chemotherapy/immunotherapy – Often combined with surgery or for advanced disease
- A lobectomy involves removing one lobe of the lung, while a pneumonectomy involves removing the entire lung.
Surgery is primarily used to treat lung cancer in early stage lung cancer or locally advanced NSCLC (typically stage I–III) when imaging shows no distant spread. Comprehensive guidance on lung cancer surgery can help patients understand where pneumonectomy fits within wider treatment options. Surgery for lung cancer may also involve the removal of nearby lymph nodes to check for cancer spread. The type of surgery you need for lung cancer depends on the size of the cancer, the position of the cancer in the lung, and the type of lung cancer. Small cell lung cancer is rarely treated with pneumonectomy because it tends to spread early and responds better to chemotherapy and radiotherapy, which are used to treat cancer.
Before recommending pneumonectomy, a multidisciplinary team (MDT) meeting reviews your case. This team includes thoracic surgeons, respiratory physicians, oncologists, radiologists, and specialist nurses. They examine your CT scans, PET-CT imaging, pulmonary function tests, and overall health to determine the best treatment path.
MDT decision-making process:
- Review of CT and PET-CT scans for tumour size, location, and spread
- Assessment of nearby lymph nodes for cancer involvement
- Lung function evaluation to predict post-operative breathing capacity
- Consideration of heart health and general fitness
- Discussion of whether lung-sparing surgery is technically possible
Pneumonectomy is often combined with other treatments. If cancer has spread to lymph nodes, adjuvant chemotherapy or immunotherapy may be recommended after surgery to reduce recurrence risk and further treat cancer.
Why might you need a pneumonectomy for lung cancer?
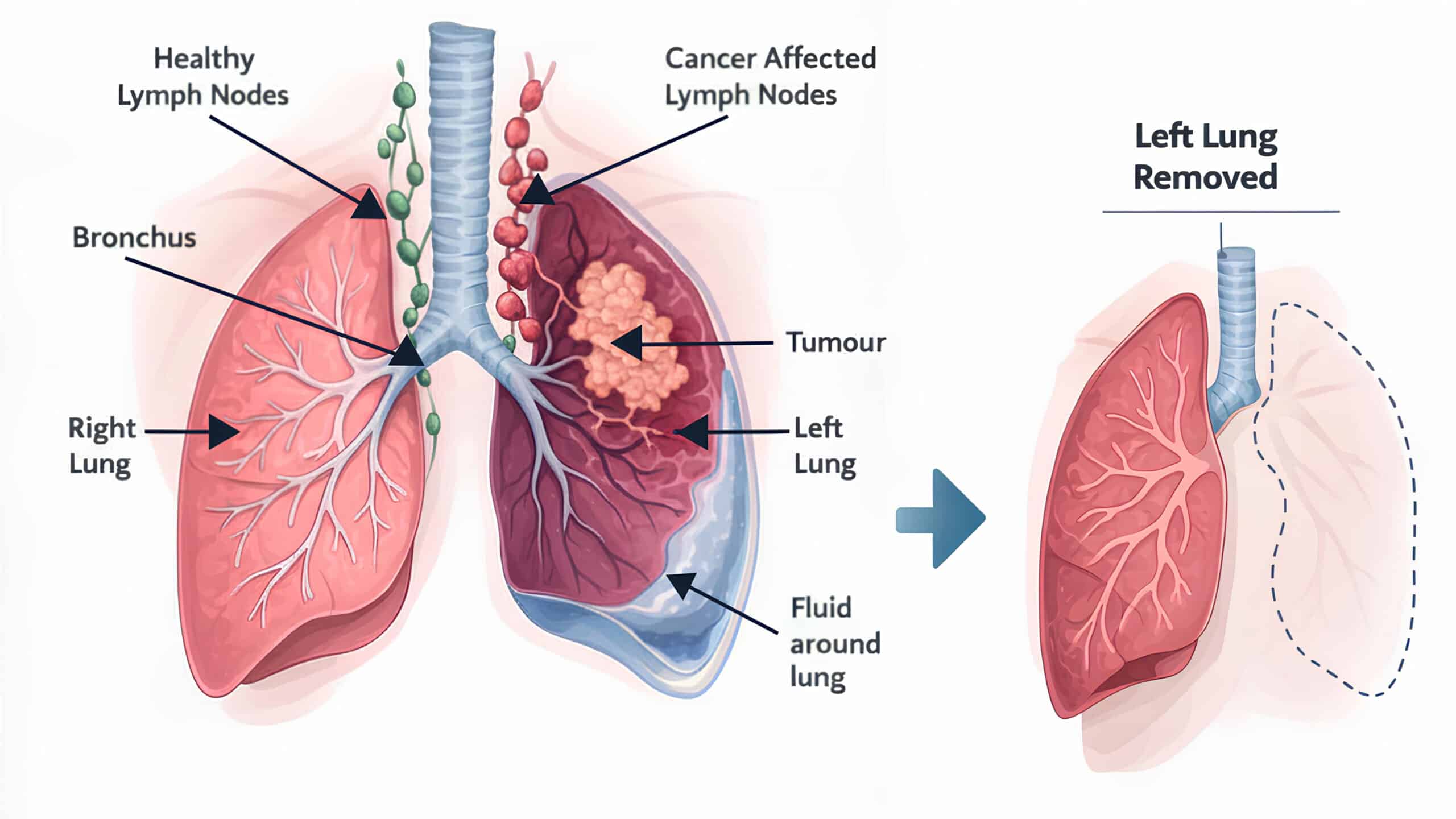
Understanding why your surgeon recommends removing the whole lung rather than a smaller portion helps you appreciate the reasoning behind this decision.
The most common scenario is a large central tumour located close to or involving the main bronchus—the major airway leading into the lung. When cancer sits at this location, removing just one lobe would leave disease behind or result in positive margins where cancer cells remain.
Other typical indications include:
- Tumours crossing fissures – When cancer extends from one lobe into another, a lobectomy alone cannot achieve clear margins
- Involvement of major blood vessels – If the pulmonary artery or veins to multiple lobes are affected, removing the entire lung may be the only way to control bleeding and clear the disease
- Tumour invasion into the main bronchus – A centrally placed tumour that cannot be reconstructed with sleeve resection techniques
Beyond lung cancer, pneumonectomy may occasionally be required for other serious chest conditions, and understanding related problems such as pneumothorax and its treatment can also be important when discussing lung surgery. Beyond lung cancer, pneumonectomy may occasionally be required for:
- Severely destroyed lung tissue from previous infections such as tuberculosis
- Extensive bronchiectasis localised to one lung
- Major traumatic injury to the lung
However, lung cancer remains by far the most frequent indication in UK practice.
Examples of tumour locations requiring pneumonectomy:
- Right main bronchus tumour extending into upper and lower lobe bronchi
- Left upper lobe tumour invading the left pulmonary artery
- Central tumour crossing the major fissure with involvement of both upper and lower lobes
Modern thoracic surgery practice favours lung-sparing operations wherever possible. Sleeve lobectomy, where a lobe and section of bronchus are removed and the airway reconstructed, preserves more lung tissue and carries lower mortality than pneumonectomy. Your surgeon will only recommend removing the whole lung when cure is unlikely without doing so.
Who is a suitable candidate for pneumonectomy?
Not every patient with lung cancer can safely undergo pneumonectomy. Careful assessment ensures that only those likely to benefit—and tolerate the surgery—are offered this complex procedure. Understanding the risk factors for lung cancer, such as smoking, environmental toxins, and asbestos exposure, is important for prevention and early detection, and these same risk factors can also influence surgical risk.
Essential criteria for candidacy:
- Cancer limited to one lung and regional lymph nodes
- No evidence of spread to liver, bones, brain, or adrenal glands on staging scans
- Adequate heart and lung reserve to function with a single remaining lung
Lung function forms a crucial part of this assessment. Your healthcare provider will arrange pulmonary function tests including spirometry and gas transfer measurements. These help calculate your predicted post-operative lung function. If your predicted values fall below certain thresholds (often cited as 30% of normal), the risks of surgery may outweigh the benefits. Your provider will also perform several tests to determine how well your heart and lungs are working before your pneumonectomy.
Heart assessments are equally important. These typically include:
- ECG to check heart rhythm
- Echocardiogram to assess heart pump function
- Cardiopulmonary exercise testing (CPET) in borderline cases to measure oxygen levels during exertion
Factors that influence risk (but don’t automatically exclude surgery):
- Age – there is no strict upper limit, but older patients may have less physiological reserve
- Previous lung disease such as COPD, emphysema, or pulmonary fibrosis
- Heart conditions including coronary artery disease or previous heart attacks
- Diabetes, kidney disease, or other chronic conditions
- Current smoking status
- Other factors such as general fitness, nutritional status, and the presence of additional comorbidities
Patients with pre-existing lung disease face a higher risk of severe breathlessness after pneumonectomy. Those with comorbidities or poor baseline health are at increased risk of complications or poorer outcomes from surgery.
Patients who smoke or are deconditioned may be offered a period of prehabilitation before surgery. This might include smoking cessation programmes, pulmonary rehabilitation, breathing exercises, and nutritional support over a few weeks to improve fitness.
In borderline situations, Mr Scarci may explore lung-sparing alternatives rather than accept the higher risks of pneumonectomy in a patient with limited reserve.
Preparing for a pneumonectomy
Thorough preparation improves outcomes and helps you feel more confident about the journey ahead.
Pre-operative consultations and tests
In the weeks before surgery, you will attend clinic appointments for detailed discussions about risks, benefits, and what to expect. An anaesthetic assessment ensures you are fit for general anesthesia. Patients must undergo extensive preoperative testing to ensure they can survive with only one functioning lung. You should arrange for time off from work for your procedure and recovery, and make transportation arrangements for your medical appointments.
Common pre-operative investigations include:
- Chest CT scan and PET-CT for detailed staging, and in many cases, a lung biopsy to confirm the diagnosis
- Brain imaging (MRI or CT) if there is any suspicion of spread
- Bronchoscopy to examine the airway and assess tumour extent
- Blood tests including full blood count, kidney function, and clotting screen
- Lung function tests (spirometry, gas transfer)
- ECG and echocardiogram for heart assessment
- Ventilation-perfusion (V/Q) scan in some cases to estimate how much each lung contributes to breathing
Medical optimisation
If you smoke, stopping at least 4–8 weeks before surgery significantly reduces your risk of complications. Your GP or hospital team can provide support with nicotine replacement or medications to help you stop smoking.
Medications may need adjusting:
- Blood thinners such as warfarin, apixaban, or clopidogrel may need to be stopped or bridged
- Some medications may be continued; your surgical team will provide specific instructions
- You will receive fasting instructions for the night before surgery
Practical home preparation
Planning ahead makes recovery easier:
- Arrange help with shopping, cooking, and housework for the first few weeks
- Plan time off work—typically 6–12 weeks depending on your job
- Organise transport to and from hospital
- Consider bed placement and mobility if stairs are difficult initially
Prehabilitation
In Mr Scarci’s London practice, both NHS and private patients receive tailored prehabilitation advice, and many people choose private thoracic surgery in London for faster access to minimally invasive treatment and personalised care. This often includes:
- Breathing exercises with an incentive spirometer
- Daily walking to build stamina
- Nutritional guidance to optimise protein intake and overall health
- Psychological support if anxiety is significant
What happens during a pneumonectomy?
Understanding each step of the operation can help reduce anxiety about this major surgery. In some cases, instead of a full pneumonectomy, an operation called a sleeve resection may be performed. This procedure removes the tumour and affected section of the bronchus, preserving more healthy lung tissue. Additional procedures, such as lymphadenectomy, may also be carried out to remove nearby lymph nodes.
During the surgery, the surgeon puts surgical instruments through small incisions in the chest, especially when using minimally invasive techniques like keyhole surgery. A drain may also be placed by the surgeon to remove fluid or air after the operation.
Video-assisted thoracoscopic surgery (VATS) is a minimally invasive approach that may be used for lung surgery, including pneumonectomy in select cases. This technique can result in less pain and a quicker recovery compared to traditional open surgery.
Day of surgery
You will be admitted either the day before or on the morning of surgery. The operating team will confirm which side (left lung or right lung) is being removed and mark this clearly. You will meet the anaesthetist who will explain the anaesthetic process.
The operation
Pneumonectomy is performed under general anesthesia. A special breathing tube allows the anaesthetist to ventilate only the unaffected lung while the surgeon operates on the other side. The operation typically takes 2–4 hours, though more complex procedure cases may take longer.
Surgical approach:
Open thoracotomy remains the standard approach for pneumonectomy. The surgeon makes a curved incision under the shoulder blade, between the ribs, to access the chest cavity. In selected cases at high-volume centres, operations may be started using video assisted thoracoscopic surgery (VATS) or robotic assisted thoracic surgery, though these minimally invasive approaches have high conversion rates to open surgery for pneumonectomy.
Main operative steps:
- The affected lung is deflated to create working space
- The pulmonary artery and pulmonary veins to that lung are carefully dissected, divided, and sealed using ligatures or staplers
- The main bronchus is divided and closed with a stapling device
- The lung removed is sent for pathology analysis
- A systematic lymph node dissection samples nearby lymph nodes to check for cancer spread
Closure and immediate post-operative measures
After removing the lung, the surgeon places one or more chest drains, commonly referred to as a chest tube, through the chest wall. The chest tube is used to drain fluid or air from the pleural space after surgery, helping to ensure proper healing and lung function. These thin tube drains also monitor for bleeding and air leak. The ribs are re-approximated, and the muscle layers and skin are closed.
You will be transferred to the recovery area or a high-dependency unit (HDU). Some patients may go to the intensive care unit (ICU) depending on their condition and the complexity of the operation.
What to expect immediately after a pneumonectomy
The first few days after surgery are closely monitored to ensure safe recovery.
Waking up
You will wake in the recovery area or HDU with several monitors attached:
- Oxygen saturation monitor on your finger
- Heart monitor (ECG) showing heart rhythm
- Blood pressure cuff for regular checks
- At least one chest drain on the operated side
- Possibly a urinary catheter and intravenous drips
Pain management
Good pain control is essential—it allows you to breathe deeply, cough effectively, and move around, all of which reduce complications.
Pain management options:
- Epidural analgesia (a thin tube in your back delivering continuous pain relief)
- Paravertebral nerve blocks
- Patient-controlled analgesia (PCA) pump allowing you to deliver measured doses of pain medication
- Transition to oral tablets as you recover
Monitoring
The nursing team will regularly check:
- Oxygen levels and respiratory rate
- Blood pressure and heart rate
- Chest drain output
- Chest X ray within the first 24 hours to confirm the remaining lung is expanding and check mediastinal position
Early physiotherapy
Physical therapy begins early. Within the first 24 hours, physiotherapists will guide you through:
- Breathing exercises to keep the remaining lung expanded
- Supported coughing techniques to protect your incision
- Sitting out of bed and beginning to mobilise
Hospital stay
Most patients stay in hospital for 7–10 days following pneumonectomy. This may be longer if complications arise. Private patients under Mr Scarci may have more flexible discharge planning once safety criteria are met.
What you will see and feel in the first 48–72 hours:
- Drips and drains attached to your body
- Oxygen via nasal prongs or mask
- Some drowsiness from medications
- Chest discomfort managed with regular analgesia
- Gradual progression from bed to chair to walking short distances
Recovery, rehabilitation, and living with one lung

Recovery from pneumonectomy is a gradual process measured in weeks and months, not days.
Short-term recovery (first month)
After discharge, focus on:
- Wound healing and pain management
- Gradually increasing walking distance each day
- Managing breathlessness by pacing activities
- Eating well to support healing
- Attending follow-up appointments
Medium-term recovery (1–3 months)
During this phase:
- Stamina improves noticeably
- Many patients return to desk-based work by 6–8 weeks
- Breathing exercises and physiotherapy continue
- Daily activities become easier, though heavy lifting should be avoided
Longer-term recovery (beyond 3 months)
Over time:
- The remaining lung adapts and expands
- The mediastinum (central chest structures) shifts to occupy the empty space
- Lung function stabilises, often reaching 70–80% of pre-operative levels in selected patients
- Most people can manage normal household activities
Typical symptoms during recovery
- Breathlessness on exertion—expected and improves gradually
- Fatigue and reduced exercise capacity initially
- Discomfort or altered sensation around the scar
- Occasional shoulder or back discomfort
Rehabilitation support
Recovery often requires several months, during which patients may need to perform breathing exercises to strengthen the remaining lung. You may tire easily after the surgery, but you will slowly start to recover your strength. Pulmonary rehabilitation programmes can significantly improve outcomes, and broader insights on lung cancer surgery highlight how rehabilitation, early diagnosis, and careful surgical planning work together to optimise recovery:
- Supervised breathing exercises
- Graded walking and aerobic exercise
- Strength training appropriate to your capacity
- Nutritional and psychological support
Practical guidance
| Activity | Typical Timeline |
|---|---|
| Driving | 4–6 weeks once you can perform an emergency stop safely |
| Flying | After surgical review; usually once chest is stable |
| Return to desk work | 6–8 weeks |
| Heavy physical work | 12+ weeks |
| Vaccinations | Annual flu vaccine and pneumococcal vaccination via GP |
| Living with one lung does mean some limitations. High-intensity sport or very heavy physical labour may not be possible. However, many patients achieve good quality of life and return to activities they enjoy. |
Risks and potential complications of pneumonectomy
Pneumonectomy is a high-risk operation. Understanding possible complications helps you prepare and make informed decisions. This surgery can lead to complications such as respiratory failure, blood clots, pneumonia, and shock. The risk of death from pneumonectomy is approximately 1 in 20, highlighting that it is considered a high-risk operation. Complications from pneumonectomy can include infection, excessive bleeding, and reactions to anesthesia. Reduced blood flow to the heart or remaining lung can also occur, which may impact recovery and overall outcomes. A broncho-pleural fistula, which is a hole in the bronchus, is another potential complication that may require additional treatment.
Mortality risk
National 30-day mortality for pneumonectomy in the UK is often quoted around 5% (approximately 1 in 20). This varies according to:
- Patient age and overall health
- Presence of co-morbidities
- Centre volume and surgical experience
- Tumour complexity
Common complications
General surgical risks:
- Bleeding requiring transfusion
- Wound infection
- Blood clots in the legs (DVT) or lungs (pulmonary embolism)—measures to prevent blood clots include compression stockings and blood-thinning injections
- Complications related to general anesthesia
Respiratory complications:
- Pneumonia in the remaining lung
- Atelectasis (partial lung collapse)
- Respiratory failure requiring prolonged oxygen support
Pneumonectomy-specific complications
Less common but significant:
- Heart arrhythmias, especially atrial fibrillation—common in the first few days
- Post-pneumonectomy pulmonary oedema—fluid overload in the remaining lung
- Air leak from the surgical site
Rare but serious:
- Bronchopleural fistula—breakdown of the bronchial stump causing air or infected fluid in the pleural space. This is one of the most feared complications
- Chylothorax—leak of lymphatic fluid into the chest
- Excessive bleeding requiring return to theatre
- Persistent chest pain or numbness due to nerve damage
- Need for prolonged ventilation, tracheostomy, or intensive care support
Risk mitigation
- Comprehensive pre-operative assessment
- Meticulous surgical technique
- Specialist post-operative care
All aim to reduce these risks. Always ask your surgeon for personalised risk estimates based on your specific situation.
Alternatives to pneumonectomy and lung-sparing options
Before committing to pneumonectomy, it is worth understanding what alternatives exist.
Lung-sparing surgical options
Where technically feasible, lung-sparing operations offer lower mortality and better post-operative lung function:
- Sleeve lobectomy – Removes a lobe plus a section of main bronchus, then the airway is reconstructed. Increasingly preferred for central tumours where anatomy allows
- Sleeve resection with vascular reconstruction – Complex but preserves lung parenchyma
- Extended lobectomy – Removes a lobe plus part of an adjacent structure
Non-surgical alternatives
For patients unfit for major surgery or who choose not to have an operation:
| Treatment | Best Suited For |
|---|---|
| SABR (stereotactic ablative radiotherapy) | Small, early-stage tumours in patients unfit for surgery |
| Chemoradiotherapy | Locally advanced disease not amenable to surgery |
| Immunotherapy/targeted therapy | Advanced NSCLC with specific mutations or PD-L1 expression |
| Radiofrequency ablation | Small peripheral tumours |
| Palliative approaches | Symptom control when cure is not possible |
Advances in minimally invasive surgery
Keyhole surgery (VATS) and robotic assisted thoracic surgery have transformed thoracic surgery. These approaches can sometimes enable complex lung-sparing resections that previously required pneumonectomy. While robotic pneumonectomy itself remains experimental with high conversion rates to open surgery, minimally invasive lobectomy and sleeve procedures are increasingly routine at high-volume centres.
Seeking a second opinion
If you have been told you need a pneumonectomy, consider asking:
- Is a lung-sparing operation feasible in my case?
- Would another centre or specialist offer different options?
- What would happen if I chose non-surgical treatment?
Specialists such as Mr Marco Scarci, who routinely perform complex and minimally invasive thoracic surgery in London, can provide additional perspectives on your options and may also advise on lung cancer screening and early detection where appropriate.
Follow-up, prognosis, and questions to ask your surgeon
Understanding what happens after surgery helps you plan for the future.
Follow-up schedule
After a pneumonectomy for lung cancer depends on your individual situation, but typically includes:
- Clinic visits every 3 months for the first 1–2 years
- Less frequent appointments (6-monthly, then annually) thereafter
- Periodic CT scans to monitor for recurrence
- Ongoing assessment of breathing, quality of life, and general health
Prognosis
Survival after pneumonectomy depends on several factors:
- Stage at surgery – Earlier stage tumours have better outcomes
- Lymph node involvement – Spread to nearby lymph nodes affects prognosis
- Margin status – Complete resection (R0) with clear margins is the goal
- Need for adjuvant treatment – Chemotherapy or immunotherapy after surgery can improve survival in appropriate cases
Many patients achieve excellent long-term survival when pneumonectomy is performed for appropriately selected, localised lung cancers.
Questions to ask your surgeon
When meeting with your surgical team, consider asking:
- Why is pneumonectomy being recommended rather than a lung-sparing operation?
- What is my personal risk of mortality and serious complications?
- How long will I be in the hospital, and will I need intensive care?
- When can I expect to return to driving, work, and normal activities?
- What support will be available after discharge—physiotherapy, home visits, specialist nursing?
- Will I need chemotherapy or other treatments after surgery?
- What are my likely long-term outcomes?
Contact Mr Marco Scarci
If you are considering lung cancer surgery in London or would like a second opinion about your treatment options, Mr Marco Scarci and his team are available for individual assessment. Consultations are offered both privately and through NHS referral pathways. Whether you need reassurance about a recommended pneumonectomy or want to explore lung-sparing alternatives, expert guidance can help you make the best decision for your health.
Understanding what lies ahead empowers you to prepare both physically and mentally for this major surgery. Reading patient testimonials about thoracic surgery can also provide reassurance about real-life recovery experiences. With specialist care and proper support, many patients go on to live full, active lives after pneumonectomy.