Receiving a lung cancer diagnosis and facing surgery can feel overwhelming. The good news is that lung cancer surgery is one of the most effective treatments for early stage disease, and the recovery process, while significant, follows a predictable path that most patients navigate successfully.
Understanding what lies ahead can ease anxiety and help you prepare. Whether you are having a wedge resection (removing a small wedge of lung tissue), a segmentectomy (removing a segment), a lobectomy (removing an entire lobe), or a sleeve resection (removing a lobe and part of the airway), the principles of recovery are similar. In each of these procedures, the surgeon removes specific parts of the lung depending on the location and size of the cancer. Lung cancer surgery typically involves removing the cancer along with some of the lymph nodes in the chest. The most common type of lung cancer surgery is a lobectomy, where the surgeon removes a lobe of the lung. A pneumonectomy involves the removal of an entire lung and is less common than other types of lung surgery. A segmentectomy is the removal of one or more segments of the lung and is recommended when a patient is not healthy enough for a lobectomy. The main difference lies in the extent of lung tissue removed and the surgical approach used.
Modern lung surgery uses two main approaches. Open chest surgery, called thoracotomy, involves a longer incision and spreading of the ribs. Minimally invasive techniques—video assisted thoracoscopic surgery (VATS) and robotic-assisted keyhole surgery—use several small incisions with a camera and specialised instruments, and resources explaining what happens immediately after a keyhole lung operation can help set expectations. Most patients having uncomplicated keyhole surgery spend approximately 2–4 days in hospital, while those having open surgery typically stay 4–7 days. Full recovery at home, meaning feeling like yourself again, generally takes 6–12 weeks.
This article focuses specifically on what happens during your recovery: from waking up after the operation, through your hospital stay, to returning home and resuming driving, work and exercise. The guidance reflects UK practice and the experience of Mr Marco Scarci, a consultant thoracic surgeon based in London who specialises in minimally invasive and robotic chest surgery techniques.
Introduction to Recovery
Recovery from lung cancer surgery is a crucial part of your overall treatment journey. Understanding what to expect during this period can help you feel more confident and prepared as you heal. Lung cancer surgery, sometimes called lung resection, is a major surgery that involves removing the cancerous part of the lung, along with some surrounding lung tissue and lymph nodes. The type of surgery you have—whether it’s minimally invasive keyhole surgery or traditional open surgery—can influence how quickly you recover and how your body heals. Most patients will need several weeks to recover from lung cancer surgery, and following your healthcare team’s instructions is essential to prevent complications and support your body as it heals. By knowing what lies ahead, you can take an active role in your recovery and give yourself the best chance for a smooth and successful outcome.
Preparation for Surgery
Preparing for lung cancer surgery is an important step in ensuring the best possible results. Before your operation, you’ll undergo a series of assessments, including heart tests and lung function tests, to help your healthcare team understand your general health and tailor your overall lung cancer surgery and recovery plan. If you smoke, stopping as early as possible is vital—smoking increases the risk of complications during and after cancer surgery. Maintaining a healthy diet and staying physically active can also help improve your lung function and reduce the risk of blood clots. Your healthcare team will guide you on how to prepare, including advice on which medications to take or stop, how to care for your wound after surgery, and when to attend follow-up appointments. Taking these steps before surgery helps set the stage for a safer operation and a smoother recovery.
Surgical Options
There are several surgical options available for treating lung cancer, and the best choice depends on the size and location of your tumour, as well as your overall health. Open surgery, or thoracotomy, involves making a large incision in the chest to access the lungs. Keyhole surgery, also known as video assisted thoracoscopic surgery (VATS), is a minimally invasive approach that uses small incisions and a camera to remove the affected lung tissue. This technique often results in less pain and a quicker recovery compared to open surgery. Open surgery, or thoracotomy, involves a larger incision to access the lung and may be necessary for more complex cases. Other procedures include wedge resection, where a small section of lung is removed, and sleeve resection, which involves removing part of the lung and reconstructing the airway. Your surgeon will discuss the most appropriate surgical option for your situation, explaining the risks and benefits of each approach so you can make an informed decision about your lung cancer surgery, including keyhole and open procedures.
Immediately After Surgery: Waking Up and Monitoring
You will wake up in the Post-Anaesthetic Care Unit, often simply called the recovery room. A nurse will be with you continuously during this time, checking your vital signs and ensuring you are comfortable as the anaesthetic wears off. After lung cancer surgery, you will wake up in the recovery room with one-to-one nursing care until you are stable enough to return to the ward.
Most patients stay in the recovery unit for a few hours before being transferred back to the thoracic ward. If you have had more extensive surgery such as a pneumonectomy (removal of an entire lung), or if you have other significant health conditions, you may spend 24–48 hours in a high dependency unit or intensive care unit for closer monitoring. This is a precaution rather than a sign that something has gone wrong.
During this early phase, you will have several monitors attached:
- Heart monitor (ECG) – sticky patches on your chest connected to a screen showing your heart rhythm
- Blood pressure cuff – automatically inflating at regular intervals
- Oxygen saturation probe – a small clip on your finger measuring oxygen levels in your blood
- Respiratory assessments – a nurse will regularly check your breathing rate and pattern
You will be positioned sitting up at about 30–45 degrees. This position helps your remaining lung tissue expand properly and reduces the risk of developing a chest infection or collapse of small airways.
It is completely normal to feel sleepy, slightly confused about the time of day, and mildly breathless straight after anaesthetic. These sensations typically improve over the first 24 hours. Some patients also experience a dry mouth and mild nausea, both of which the nursing team can address with fluids and medication.
Mr Scarci’s healthcare team will keep your family informed about your progress and let them know when visiting is appropriate—usually from day one, once you are settled on the ward.
Tubes, Drains and Oxygen
Waking up with tubes and lines attached to your body is entirely normal after chest surgery. It can look alarming, but each serves an important purpose and most are removed within a few days.
Here are the common tubes you may have:
| Tube/Line | Purpose | Typical Removal Time |
|---|---|---|
| Chest drain(s) | Removes air and fluid drainage from around the lung so it can re-expand | 2–3 days (VATS); up to 5–7 days (open surgery) |
| Intravenous (IV) line | Provides fluids and medications | When eating and drinking normally |
| Arterial line (wrist) | Allows precise blood pressure monitoring and blood gas sampling | Usually within 24–48 hours |
| Urinary catheter | Measures how much urine you produce while less mobile | Day 1–2 |
| Central line (neck) | Supports more complex cases with medication infusions | Only used when needed; removed before discharge |
| The chest drain is the most important device after lung surgery. This thin tube exits through your chest wall and connects to a clear collection bottle or Portex bag system. You will notice bubbling and fluid collecting—this is entirely normal and shows the drain is working. The drain stays in place until air leak stops and fluid output drops to a safe level, usually below 100–200 mL per day. |
You will also receive oxygen through nasal prongs or an oxygen mask in the first hours to days after surgery. Your nurse will monitor your oxygen levels closely and gradually wean you off supplemental oxygen as your breathing improves. Coming off oxygen completely is an important early recovery milestone for most patients.
Pain Control and Comfort
It is normal to have some soreness or pain for the first week or so after lung cancer surgery.
Good pain control is essential for your recovery. When pain is well managed, you can take deep breaths, cough effectively, participate in physiotherapy, and start walking—all of which dramatically reduce your risk of complications such as pneumonia and blood clots.
Do not try to “put up with” severe pain. Speak up early if your pain is not controlled, as there are many effective options available.
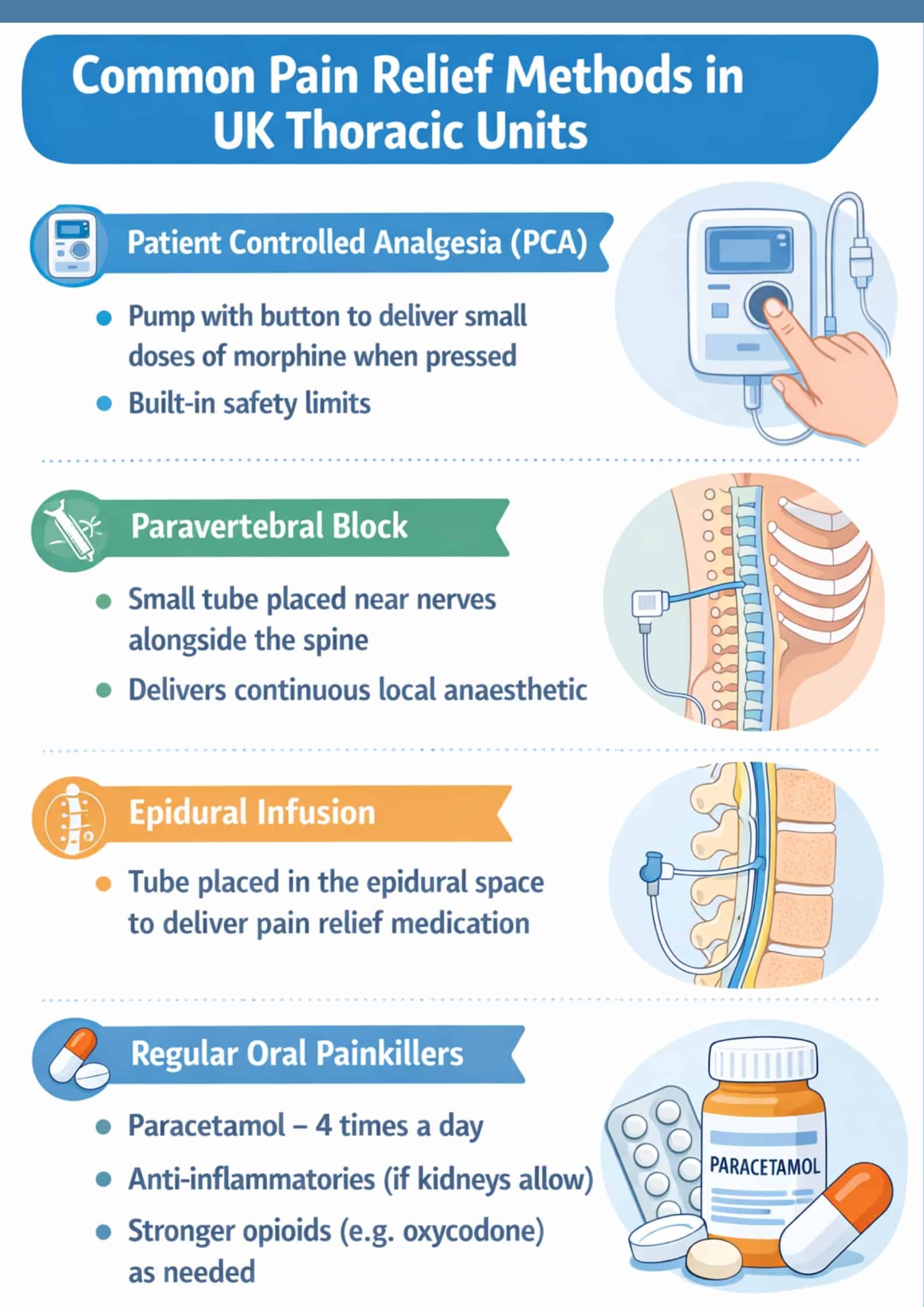
Common pain relief methods in UK thoracic units include:
- Patient controlled analgesia (PCA) – A pump with a button that delivers small doses of morphine when you press it. The system has safety features to prevent overdose.
- Paravertebral block – A small tube placed near the nerves alongside your spine, delivering continuous local anaesthetic.
- Epidural infusion – Similar to paravertebral, sometimes used for open surgery.
- Regular oral painkillers – Paracetamol four times daily, anti-inflammatory tablets if your kidneys allow, and stronger opioids such as oxycodone as needed.
Painkillers may be provided through a small tube called a paravertebral catheter while you are in the hospital.
Your nursing team will regularly ask you to rate your pain on a 0–10 scale and adjust your medication accordingly. Aim for a pain score below 4 out of 10, which allows you to move and breathe comfortably. You will be given painkillers to manage your pain after lung cancer surgery. It is important to tell your doctor or nurse as soon as you feel any pain after surgery.
Some patients experience burning or stabbing nerve pain along the incision site. This is caused by irritation of the intercostal nerves between the ribs and usually improves over 4–6 weeks. Medications such as gabapentin can help if this becomes bothersome.
Simple comfort measures make a real difference:
- Hold a small pillow against your wound when coughing to reduce discomfort
- Use extra pillows to support yourself at night
- Do gentle shoulder rolls and arm movements to prevent stiffness on the operated side
You will be given a one-week supply of painkillers to take home after your surgery. You should contact your doctor if your pain continues for more than a few weeks after surgery.
Your Surgical Wound and Chest Drains
The appearance of your surgical wound depends on the technique used. Keyhole surgery leaves 3–4 smaller wounds of about 1–3 cm each. Open thoracotomy leaves a single longer incision, typically 10–20 cm, curving around the side of your chest. You may have several tubes or drains after surgery, including a chest drain to help your lung expand again.
Dressings are usually removed or changed 24–48 hours after surgery so the team can inspect the incision site. If the wound is dry and healing well, lighter dressings are applied. Many modern wounds use dissolvable stitches placed beneath the skin, meaning there is nothing to remove. If clips or staples are used, your district nurse or practice nurse will remove them 7–10 days after surgery.
Normal healing sensations include:
- Tightness around the scar
- Itching as the wound heals
- Numb patches around the incision (this occurs because small nerves are cut during surgery and may take 3–6 months to recover)
Most wounds heal well without problems. However, you should contact the hospital, your GP, or Mr Scarci’s team immediately if you notice:
- Increasing redness spreading from the wound
- Swelling or heat around the incision
- Discharge (especially if cloudy or smelly)
- Fever above 38°C
A small number of patients are discharged home with a chest drain still in place for ongoing fluid drainage. If this applies to you, you will receive specific written instructions and regular visits from community nursing staff to manage the drain safely.
Getting Moving: Physiotherapy, Breathing and Early Activity
Early movement is one of the most important parts of modern post-surgery recovery programmes for lung cancer. Getting up and moving reduces your risk of chest infection, blood clots, and prolonged weakness.
A physiotherapist will visit you on the first day after surgery, often within hours of your return to the ward. They will teach you deep breathing exercises and coughing techniques to clear secretions from your lungs. Many patients use an incentive spirometer or similar device—a simple gadget that encourages you to take slow, deep breaths and shows you how well you are doing.
Typical activity milestones during your hospital stay:
- Within 12–24 hours: Sitting on the edge of the bed, then transferring to a chair
- Day 1–2: Walking a few steps with help from staff
- Day 2–3: Walking along the ward corridor (starting with 10–50 metres)
- Before discharge: Walking independently to the bathroom and back
While in bed, you will be encouraged to do simple exercises such as ankle pumps and leg movements every hour. These help maintain blood flow and prevent blood clots forming in your leg veins. You may also receive daily injections of blood-thinning medication (such as enoxaparin) and wear compression stockings until you are fully mobile.
Shoulder and arm exercises on your operated side are equally important. The physiotherapist will show you gentle movements to prevent the shoulder becoming stiff—a complication that affects about 1 in 10 patients who remain immobile.
Eating, Drinking and Bowel Function
Your appetite may be poor in the first few days after surgery. This is normal, but good nutrition helps your body heal and supports your immune system. It is recommended to eat a balanced diet with high energy foods to support recovery after lung cancer surgery.
Most patients can start sipping water a few hours after waking from anaesthetic, progressing to eating and drinking light meals the same day or the next morning depending on how they feel. Anti-sickness medication is available if nausea is a problem. Patients are advised to drink at least 2 liters of fluid daily to prevent constipation post-surgery.
Practical nutrition tips:
- Choose high-protein foods (eggs, chicken, fish, beans, dairy) to support tissue repair
- Eat small, frequent meals rather than three large ones
- High-calorie options may be helpful if you have lost weight before surgery
- A dietitian may become involved if you have significant weight loss or frailty
Constipation is extremely common after surgery, affecting up to 70% of patients. This happens because opioid painkillers slow the bowel and you are less active than usual. Prevention is much easier than treatment:
- Drink 1.5–2 litres of fluid daily unless your medical team advises otherwise
- Include fibre-rich foods such as fruit, vegetables, and wholegrain bread
- Take the prescribed laxatives regularly—don’t wait until you are already constipated
If you have not had a bowel movement for several days despite laxatives, or if you develop persistent nausea or vomiting, let your healthcare team or GP know promptly.
Preventing Complications
Preventing complications is a key focus during your recovery from lung cancer surgery. Your healthcare team will work closely with you to reduce the risk of issues such as blood clots, chest infection, and wound infection. Simple steps like performing deep breathing exercises and getting up and moving as soon as possible after surgery can help maintain lung function and prevent chest infection. To prevent blood clots, you may be given blood-thinning medication and encouraged to do gentle leg exercises. Proper wound care is also essential to avoid infection and support healing. Your healthcare team will provide clear instructions and monitor your progress, helping you recognise any warning signs early. By following their advice and staying engaged in your recovery, you can minimise risks and support your body as it heals after lung cancer surgery.
You will receive instructions on how to care for your wound before you leave the hospital.
Recovery Timeline
Recovery from lung cancer surgery is a journey that unfolds over several weeks, with each stage bringing new milestones and improvements. Immediately after your cancer surgery, you will spend the first few days in hospital, where your healthcare team will closely monitor your oxygen levels, blood pressure, and overall health. This initial hospital stay is crucial for managing pain, preventing blood clots, and ensuring your lung is healing as expected.
Once you are stable and able to move around safely, you will be discharged to continue your recovery at home. The first few weeks at home are often marked by gradual progress—most patients notice they feel tired and need to rest frequently, but each day brings small improvements in strength and lung function. During this period, it’s essential to follow your healthcare team’s advice, including taking prescribed medications, performing deep breathing exercises, and attending follow-up appointments. These steps help prevent complications such as blood clots and support your body as it heals.
Patients who have undergone minimally invasive keyhole surgery (such as video assisted thoracoscopic surgery) often recover faster, with a shorter hospital stay and less pain compared to those who have had open chest surgery. However, regardless of the surgical approach, it’s normal for recovery to take several weeks. Most patients can expect to gradually return to light activities within a few weeks, with a full return to normal routines taking a bit longer, depending on the extent of surgery and individual health.
Throughout your recovery, your healthcare team will check your progress, monitor your oxygen levels, and ensure your pain is well controlled. By staying active with gentle movement, following advice to prevent blood clots, and keeping up with deep breathing exercises, you can help your lungs recover faster and reduce the risk of complications. Remember, every patient’s recovery timeline is unique, but with patience and support, most people regain their strength and independence after lung cancer surgery.
Leaving Hospital and the First Weeks at Home
Most patients having uncomplicated keyhole surgery are ready to leave hospital after 2–4 days. Those having open thoracotomy typically stay 4–7 days. Your exact hospital stay depends on how quickly you meet the discharge criteria.
Before you can go home, the team will check:
- Your breathing is safe on room air (or low-flow oxygen if arranged)
- Your observations (heart rate, blood pressure, temperature) are stable
- You can get to the bathroom with minimal help
- Pain is controlled with tablets
- You have appropriate support at home
Fatigue is the most common complaint in the first week and often continues for several weeks after your surgery. This is completely normal—your body is using energy to heal. The key is to pace yourself: do a little activity, then rest, rather than pushing through until exhausted.
Practical arrangements for the first 1–2 weeks at home:
- Ask someone to help with shopping, cooking, and cleaning
- Consider having a family member or friend stay with you initially
- Arrange transport to any follow up appointments (you will not be able to drive yet)
- Keep your discharge paperwork and emergency contact numbers somewhere easy to find
A sensible activity progression looks like this:
| Week | Activity Level |
|---|---|
| 1–2 | Walking around the house several times daily; climbing stairs once or twice |
| 3–4 | Short outdoor walks (10–20 minutes); climbing stairs more confidently |
| 5–6 | Gradually increasing walking distance and pace |
| Patients under Mr Scarci’s care receive personalised written discharge instructions and 24/7 contact numbers for urgent concerns, which can be especially valuable for those choosing private thoracic surgery in London. | |
Breathing, Coughing and Lung Function During Recovery
It is normal to feel tired and more short of breath than usual for a while after losing part of a lung. Your body needs time to adapt, and the remaining lung tissue gradually expands to fill more of the chest space. Most patients find their breathing improves steadily over weeks to months.
Continue your deep breathing exercises at home—aim for 5–10 slow, deep breaths every hour while awake during the early weeks. Use any devices you were given, such as an incentive spirometer, to track your progress. Incentive spirometer should be used 5-10 times an hour after lung surgery to prevent lung collapse. Practicing deep breathing and huffing hourly after surgery is important for clearing mucus and ensuring lung function.
A dry or slightly productive cough is common after lung resection and usually settles within 4–8 weeks. However, certain symptoms require urgent medical review:
- Coughing up fresh blood (more than streaks)
- Large amounts of thick or discoloured phlegm suggesting chest infection
- Sudden severe breathlessness that does not improve with rest
Your follow-up appointments may include a chest x ray and lung function tests to assess how well your remaining lung is working. Research shows that forced vital capacity drops by 20–30% immediately after lobectomy but typically recovers to 70–90% of predicted values by three months.
Smoking and lung recovery
If you smoke, stopping before and after surgery significantly improves your lung function recovery—by 20–30% according to NHS data. It also reduces your risk of complications and cancer recurrence. Ask your healthcare team about NHS smoking cessation services or private support programmes if you need help to stop smoking.
Driving, Work, Exercise and Daily Activities
The timing of your return to normal activities depends on several factors: the type of surgery depending on extent, your general health, and the physical demands of your work and hobbies.
Driving
Most patients can consider driving again around 4–6 weeks after lung surgery, you should consult your doctor about when it is safe to resume driving after lung cancer surgery, as it can vary based on individual recovery.. Before getting behind the wheel, you should be able to:
- Wear a seatbelt comfortably without pain
- Perform an emergency stop confidently
- Turn to check mirrors and blind spots
- No longer be taking strong opioid painkillers that cause drowsiness
Check with your surgeon that they are happy for you to drive, and inform your car insurance company that you have had surgery.
Work
Return to work varies considerably:
- Desk-based jobs: Often possible from 4–8 weeks
- Manual or physical roles: Usually 8–12 weeks or longer
- Heavy lifting occupations: May require modifications or longer recovery
A phased return (starting part-time or with lighter duties) often works well. Discuss timing at your follow up appointment.
Exercise
Walking is the best form of exercise in early recovery. Start with short walks around the house, then slowly build up to 20–30 minute outdoor walks by week 4–6. Aim to gradually increase your step count, working towards around 5,000 steps daily by week 3 if comfortable. You should avoid heavy lifting, pulling, or pushing for 2 to 4 weeks after surgery to allow your body to heal properly.
Avoid:
- Heavy lifting (more than 5kg) for at least 4–6 weeks
- Strenuous gym workouts for 6–12 weeks
- Contact sports until cleared by your surgeon

Daily activities and intimacy
Gentle household tasks can be resumed gradually as your stamina improves. Sexual activity can restart when you feel comfortable and pain is controlled—typically after 2–4 weeks. Avoid positions that put strain on your chest or incision. It is important to gradually increase your physical activity after lung cancer surgery, starting with short walks and building up over time.
Patients who have had a full pneumonectomy, or who have heart disease or other significant conditions, should follow bespoke guidance from their consultant, as recovery timelines may be longer.
Lifestyle Changes After Lung Cancer Surgery
Adopting healthy lifestyle changes after lung cancer surgery is key to supporting your recovery and protecting your long-term health. One of the most important steps you can take is to stop smoking if you haven’t already—quitting smoking not only improves lung function but also reduces the risk of cancer recurrence and other complications. Your healthcare team can connect you with resources to help you quit for good.
Maintaining a balanced diet rich in protein, vitamins, and minerals will help your body heal and boost your immune system. Regular, gentle physical activity—such as short walks or light stretching—can help you recover faster, improve your lung function, and reduce the risk of blood clots. It’s important to avoid heavy lifting, strenuous exercise, or bending for several weeks after surgery to protect your healing lung and incision.
To further prevent blood clots, your team may recommend wearing compression stockings and taking prescribed blood-thinning medication. Managing pain is also crucial; take your pain medication as directed and don’t hesitate to ask for adjustments if you’re uncomfortable. Keeping your wound clean and dry, and watching for signs of wound infection, will help ensure a smooth recovery.
You may need to adjust your daily routine by taking regular breaks to rest, pacing your activities, and gradually increasing your level of physical activity as you feel stronger. Attending all follow-up appointments and communicating any concerns with your healthcare team will help you stay on track. By making these lifestyle changes and following your team’s advice, you can support your recovery from lung cancer surgery and lay the foundation for better health in the future.
Follow-Up Appointments and Ongoing Cancer Treatment
Your first outpatient follow up appointment is usually scheduled 2–6 weeks after surgery with the thoracic surgeon or lung cancer team. During follow-up appointments, your doctor will check your recovery and discuss any further treatments you may need. You should contact your doctor or nurse if you notice any new symptoms between follow-up appointments. It is important to write down any questions you have before your follow-up appointment to help you remember what to ask. You may need to return to a nurse-led clinic for assessment of wounds or drainage systems after your surgery. If you are discharged with a chest drain, a district nurse may be arranged to visit you at home for care.
What happens at this visit:
- Review of pathology results from the removed lung tissue and lymph nodes. Your surgeon will give you the results of the surgery during your follow-up appointment.
- Discussion of final cancer staging and what it means for your prognosis
- Examination of your wound and assessment of your breathing
- Opportunity to ask questions about recovery or new symptoms
Depending on the findings, some patients will be referred to an oncologist to discuss further treatment. Chemotherapy is recommended for approximately 20–30% of patients with stage II or III disease. Others may need immunotherapy, targeted therapy, or radiotherapy depending on the type of cancer cells found (such as non small cell lung or small cell lung cancer).
Beyond the initial appointment, you will have ongoing surveillance, typically involving CT scans or chest x rays at defined intervals over months and years. This monitoring helps detect any recurrence early, when treatment is most effective. How often you have check-ups after your initial follow-up appointment depends on the results of your surgery.
When to contact the team between appointments:
- Persistent cough lasting more than expected
- Unexplained weight loss
- New chest pain or breathlessness
- Any other new symptoms that concern you
Do not wait for your next scheduled appointment if something feels wrong.
Mr Scarci offers both in-person and virtual consultations in London for UK and international patients, making it convenient to review your recovery and discuss next steps wherever you are based with support from his multidisciplinary thoracic team.
Your Mental and Emotional Recovery
Lung cancer surgery affects far more than your body. It is completely normal to experience emotional ups and downs during recovery—your mind is processing a significant event. Key challenges in recovery from lung cancer surgery include severe fatigue, persistent pain, breathlessness, and potential emotional distress.
Common experiences in the weeks and months after surgery:
- Feeling tearful or emotionally sensitive
- Anxiety about cancer recurrence
- Frustration with fatigue and physical limitations
- Changes in body image related to scars
- Difficulty sleeping or concentrating
These reactions do not mean you are weak or failing to cope. They are a normal part of adjusting to what you have been through.
Talk openly with your partner, family, and healthcare team about how you are feeling. If low mood, anxiety, or fear of recurrence persist beyond the first few weeks, professional psychological support can make a real difference. Studies show that cognitive behavioural therapy reduces anxiety and depression symptoms by up to 40% in post-surgery cancer patients.
Sources of support in the UK:
- Your specialist nurse or lung cancer clinical nurse specialist
- Hospital psychology or counselling services
- Macmillan Cancer Support (phone line and local centres)
- Maggie’s Centres (free drop-in support at many UK hospitals)
- Patient support groups for people who have had lung cancer surgery
Mr Scarci’s team can signpost patients to appropriate local and national support services as part of holistic care, and many people find reassurance in reading patient testimonials about their thoracic surgery experience.
When to Seek Urgent Medical Help
While most patients recover without complications, certain symptoms always need urgent assessment. Keep this information somewhere accessible and do not hesitate to act if needed.
Call 999 or go to A&E immediately for:
- Sudden severe breathlessness
- Severe chest pain not relieved by rest or medication
- Coughing up significant amounts of fresh blood
- Signs of stroke (face drooping, arm weakness, speech difficulty)
- Confusion or marked drowsiness
Contact the thoracic ward, Mr Scarci’s team, or your GP urgently for:
- High fever (above 38.5°C) or chills
- Rapidly worsening redness, swelling, or discharge from your wound (possible wound infection)
- Calf pain, swelling, or redness (possible blood clot in leg)
- Chest pain that is worsening or different from your usual post-operative discomfort
Your written discharge paperwork includes specific phone numbers for urgent concerns. Keep these details handy at all times—by your bed, in your wallet, and saved in your phone.

How Mr Marco Scarci and His Team Support Your Recovery
Mr Marco Scarci is a consultant thoracic surgeon based in London with extensive experience in cancer surgery, including complex lung cancer operations. His practice focuses on minimally invasive techniques—VATS and robotic surgery—where these approaches are appropriate for the individual patient.
Benefits of minimally invasive lung surgery include:
- Smaller wounds with less pain
- Shorter hospital stay (often 2–3 days less than open surgery)
- Faster return to normal activities
- Reduced risk of complications such as wound infection and prolonged pain
The typical care pathway includes thorough pre-operative assessment and optimisation of your general health, clear explanation of your operation and what to expect, enhanced recovery programme protocols on the ward, and a tailored discharge plan with follow-up arrangements across the range of thoracic conditions Mr Scarci treats, including lung cancer.
Blood transfusions are rarely needed with modern techniques, and heart tests are performed beforehand when indicated to ensure safety. The intensive care unit is available for patients who need closer monitoring, but most patients recover faster on the dedicated thoracic ward.
Both face-to-face and virtual consultations are available for pre-operative counselling and post-operative review. This flexibility is especially helpful for patients travelling from outside London or from overseas who want to discuss their case before committing to surgery, or who need convenient follow-up without repeated journeys.
If you are considering lung cancer surgery, seeking a second opinion, or want to understand your recovery options in more detail, arranging a consultation with Mr Scarci is a straightforward next step. His team can review your scans, discuss the surgical options including keyhole surgery approaches, and provide honest guidance about what recovery will look like for your specific situation.
Recovery from lung cancer surgery takes time, patience, and the right support. With modern surgical techniques, enhanced recovery protocols, and expert care, most patients return to their daily lives within weeks to months. The journey is not always easy, but understanding what to expect at each stage makes it more manageable.
If you have questions about lung cancer surgery or would like to discuss your individual case, contact Mr Marco Scarci’s team to arrange a consultation.
Conclusion
Lung cancer surgery marks a major milestone in your treatment journey, and understanding the recovery process is essential for achieving the best possible outcome. Careful preparation, clear communication with your healthcare team, and a commitment to following post-operative advice all play a vital role in your recovery after lung surgery.
Staying informed about your lung cancer diagnosis and the different types of lung cancer surgery—such as keyhole surgery and open chest surgery—can help you make confident decisions about your care. It’s important to be aware of the potential risks, including blood clots, chest infection, wound infection, and the rare need for blood transfusions. Knowing how your body is monitored after surgery—through checks of your blood pressure, oxygen levels, and the use of a chest drain—can help you feel more in control and prepared for each stage of recovery.
The enhanced recovery programme, which includes patient-controlled analgesia for pain control, early mobilisation, and deep breathing exercises, is designed to help you recover faster and reduce complications. Your healthcare team—including specialist nurses and district nurses—will support you both in hospital and at home, ensuring you have the guidance and care you need as your wounds heal and your strength returns.
Mental and emotional well-being are just as important as physical healing. Don’t hesitate to reach out for support, whether through your healthcare team, support groups, or helplines. As you recover over several weeks, focus on slowly building up your activity levels, resuming normal activities at your own pace, and watching for any new symptoms that may arise.
By taking an active role in your recovery, attending all follow-up appointments, and working closely with your healthcare team, you can optimise your chances of a smooth recovery and a return to a fulfilling life after lung cancer surgery. Remember, patience and persistence are key—each step forward brings you closer to regaining your health and independence.