Introduction
Lung cancer progression varies dramatically depending on the type of cancer, ranging from aggressive doubling in weeks to slow growth over years. Understanding this timeline is essential for making informed decisions about when surgical intervention or lung cancer treatment offers the best chance of cure. Early detection and strategies to diagnose cancer, such as screening with lung CT scans, are crucial for improving outcomes. Additionally, cancer prevention and risk reduction remains important for those at increased risk.
This article covers progression rates for different types of lung cancer, explains how cancer staging affects surgical options, and outlines the factors that influence treatment timing. It is written for people diagnosed with suspected or confirmed lung cancer, their families, and anyone seeking clarity before consulting a thoracic surgery specialist. The prognosis depends on individual factors such as cancer type, stage at diagnosis, overall health, and access to treatment. Whether you have received a recent lung cancer diagnosis or are researching options for a loved one, this information will help you understand what to expect and what questions to ask your healthcare provider.
Direct answer: Lung cancer progress depends primarily on whether you have small cell lung cancer (SCLC) or non-small cell lung cancer (NSCLC). SCLC typically doubles in volume every 30-90 days and requires urgent treatment, while NSCLC subtypes often progress over months to years. Surgery and other lung cancer treatment options are typically considered for stages of lung cancer I–III when the tumour is technically resectable, and the patient is medically fit.
After reading this article, you will understand:
- How quickly different lung cancer types grow and spread
- What the TNM or Tumor (size/extent), Node (spread to lymph nodes), and Metastasis (spread to other body parts) staging system means for your treatment options
- Which factors accelerate or slow lung cancer progression
- When surgery or lung cancer treatment becomes necessary, what determines candidacy
- How to navigate common challenges in managing progression
Understanding Lung Cancer Progression
Lung cancer progression refers to how cancer cells grow, multiply, and potentially spread from the original tumour site to lymph nodes and distant organs. This process determines both prognosis and treatment options, making it central to every conversation about lung cancer care, including decisions about lung cancer surgery for diagnosis and recovery.
When lung cancer cells develop, they initially form a single tumor in the lung tissue. These cancerous cells may invade nearby structures, enter the lymphatic system or blood vessels, and establish secondary tumours elsewhere in the body. Lung cancer spreads to parts of the body such as lymph nodes, bones, brain, liver, adrenal glands, and other organs, leading to metastatic cancer. The speed at which this happens varies enormously based on cancer type, tumour biology, and individual patient factors.
Types of Lung Cancer and Their Growth Rates
There are two main types of lung cancer: non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC). NSCLC accounts for approximately 80% to 85% of lung cancer cases, while SCLC accounts for about 10% to 15%.
Small cell lung cancer accounts for approximately 10-20% of lung cancer cases and is the most aggressive form. Research shows SCLC has a volume doubling time of approximately 30-90 days, meaning the tumour can double in size within one to three months. This rapid progression explains why SCLC is often discovered at an extensive stage, when the cancer has spread beyond the chest. Like lung cancer, other cancers, such as breast cancer, can also progress to advanced or metastatic stages, requiring different treatment approaches.
Non-small cell lung cancer represents 80-90% of cases and includes several subtypes with different growth characteristics. Adenocarcinoma, the most common subtype, has a mean volume doubling time of approximately 200-250 days for solid tumours. Squamous cell carcinoma tends to grow faster, with doubling times around 140 days. Part-solid and ground-glass nodules, often representing early lung cancer, may take over 500 days to double, sometimes allowing for careful surveillance before intervention.
The connection between cancer type and surgical urgency is direct: fast lung cancer types like SCLC rarely present opportunities for surgical cure, while slower-growing NSCLC subtypes often remain surgically treatable for extended periods if diagnosed early.
The TNM Staging System and Progression Markers
The TNM system is the standard method for staging lung cancer, providing a standardised framework for describing how far lung cancer has spread. Understanding this system helps patients grasp why certain treatments are recommended at specific times.
Lung cancer stages range from 0 to 4, with stage 0 indicating the presence of abnormal cells that have not spread, and stage 4 indicating advanced cancer that has metastasized to other organs.
T (Tumour) describes the primary tumour’s size and whether it has invaded local structures or involves multiple tumour nodules within the same lobe. A T1 tumour measures 3cm or less, while T4 indicates invasion of critical structures like the heart or major blood vessels, or spread to the other lung.
N (Nodes) indicates whether cancer has spread to nearby lymph nodes, including those on the same side of the chest. N0 means no nodal involvement, while N3 indicates spread to lymph nodes inside the chest on the opposite side or above the collarbone.
M (Metastasis) confirms whether the cancer has spread to distant organs such as the brain, liver, bones, adrenal glands, or the other lung. M0 means no distant spread; M1 indicates metastatic lung cancer.
These elements combine to determine overall lung cancer stages, with higher stages indicating more extensive spread, including to the same lobe, same side, or even the other lung:
- Stage I: Small tumour confined to one lung, no lymph node involvement
- Stage II: Larger tumour or spread to nearby lymph nodes within the same lung, or multiple tumour nodules within the same lobe
- Stage III: Locally advanced disease involving lymph nodes in the central chest or on the same side, and may include multiple nodules in the same lobe
- Stage IV: The most advanced stage, where cancer has spread to distant organs or the other lung
Surgery offers curative potential primarily in stage I, stage II, and selected stage III cases. Understanding your stage directly informs your treatment plan and timeline.
Factors That Influence Progression Speed
Tumour Biology and Genetic Factors
Genetic changes within cancer cells significantly influence how aggressively a tumour behaves. Mutations in genes such as EGFR and ALK rearrangements may indicate tumours that respond well to targeted therapies. In contrast, KRAS and TP53 mutations often correlate with more aggressive disease and faster progression.
Tumour grade (how abnormal cells appear under microscopy) also matters. Poorly differentiated (high-grade) tumours typically grow faster and have higher metastatic potential than well-differentiated cancers. SCLC is inherently high-grade, explaining its rapid doubling time.
Angiogenesis, the formation of new blood vessels to supply the tumour, accelerates progression by providing cancer cells with nutrients and pathways for spread. Tumours with high angiogenic activity and early vascular invasion tend to metastasise sooner.
Patient Health and Environmental Factors
Age and overall health influence both progression and treatment options. While younger patients may develop more aggressive tumours, they often tolerate surgery better than older patients with multiple comorbidities.
Smoking status remains the leading risk factor for aggressive lung cancer. Active smoking accelerates progression, while quitting smoking, even after diagnosis, may slow disease advancement and improve surgical outcomes. The immune system also plays a role; immunocompromised patients may experience faster progression due to reduced surveillance of abnormal cells.
Comorbidities including chronic obstructive pulmonary disease, heart disease, and poor nutritional status affect both cancer behaviour and whether a patient can safely undergo surgery. These other factors must be carefully weighed when planning treatment.
Early Detection vs Late Diagnosis Impact
Early lung cancer is typically asymptomatic, which explains why many patients are diagnosed only when the cancer has advanced. As lung cancer progresses from localized, asymptomatic tumors to regional spread and distant metastasis, symptoms begin to appear. Common symptoms of lung cancer include:
- Persistent cough
- Chest pain
- Shortness of breath (breathlessness)
- Coughing up blood or rust-colored phlegm (blood in phlegm)
- Significant fatigue
- Unexplained weight loss
Lung cancer symptoms such as persistent cough, blood, chest pain, shortness of breath, and unexplained weight loss often develop only after the tumour has grown substantially or spread.
Screening programmes using low-dose CT scans identify cancers at earlier stages, when they are smaller and more likely to be surgically curable. Studies show that screen-detected cancers have similar doubling times to clinically detected cancers, but they are caught at stages where surgery can destroy cancer cells before they spread. Recent research and guidelines published in the European Journal of Cancer Prevention further support the importance of lung cancer screening for early detection in the UK, demonstrating improved survival rates and outcomes when lung cancer is diagnosed at an early stage.
Diagnostic delays compound the problem. In the UK, data shows that patients may wait over 80 days from referral to surgery for stage I/II NSCLC, well above the recommended 49-day target. For every four weeks of treatment delay, mortality risk increases by 6–13% in lung cancer settings. This underscores why prompt specialist referral and expedited staging matter significantly.

When Surgical Intervention Becomes Necessary
Surgical resection remains the primary curative treatment for early stages of lung cancer. Understanding when surgery is appropriate and when it is not helps patients navigate complex treatment decisions.
Criteria for Surgical Candidacy
Surgery offers the best curative potential when cancer is confined to the chest without distant metastases. The multidisciplinary team, comprised of thoracic surgeons, respiratory physicians, oncologists, and radiologists, evaluates several factors:
Medical fitness: Pulmonary function tests (FEV1, DLCO) must confirm adequate lung reserve to tolerate removal of lung tissue. Cardiac assessment ensures the patient can withstand surgery. Performance status (how well patients manage daily activities) strongly predicts surgical outcomes.
Tumour location and resectability: Peripheral tumours in one lung are more accessible than central tumours involving major blood vessels or airways. Involvement of critical structures may preclude complete resection with negative margins.
Staging limitations: Surgery is generally not indicated when imaging tests confirm distant metastases (stage IV) or extensive mediastinal lymph node involvement (certain stage III cases). Complete staging, including PET-CT, brain MRI, and sometimes mediastinal lymph node sampling via EBUS, must be completed before surgical planning.
Histology and molecular profile: While NSCLC is the primary surgical disease, SCLC surgery is reserved for extremely rare cases of very early, node-negative disease. Molecular testing may influence whether neoadjuvant therapy (treatment before surgery) is recommended.
Optimal Timing for Different Stages
| Stage | Surgical Urgency | Typical Timeline | Considerations |
|---|---|---|---|
| Stage I | High priority | Within 4–6 weeks of diagnosis | Delays beyond 40 days increase mortality; expedited pathway essential |
| Stage II | High priority | Within 4–6 weeks of diagnosis | May require systematic staging to exclude occult nodal disease |
| Stage III | Case-dependent | After multidisciplinary review | Often requires neoadjuvant chemotherapy or chemoradiation before surgery |
| Stage IV | Surgery rarely indicated | Focus on systemic therapy | Palliative procedures may relieve symptoms but do not cure |
| Limited-stage SCLC | Surgery extremely rare | Immediate systemic therapy standard | Surgery only for highly selected cases with no nodal involvement |
UK national targets recommend treatment within 49 days of first specialist consultation, with decision-to-treat to treatment start within 21 days. Current data shows actual waiting times averaging 83 days for surgical cases, a gap that directly impacts outcomes.
Minimally Invasive Surgical Approaches
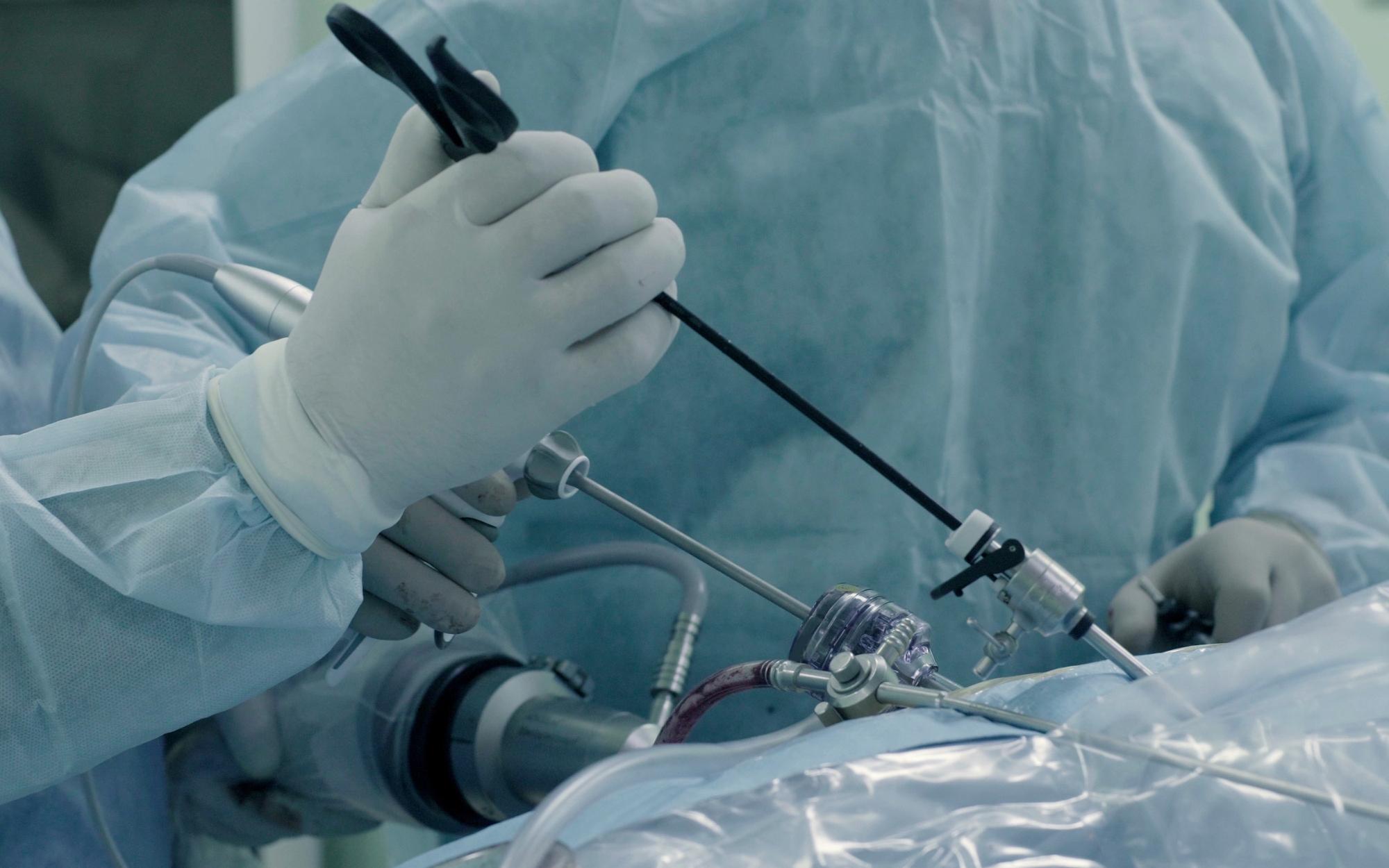
Video-Assisted Thoracoscopic Surgery (VATS) has become the standard approach for early-stage NSCLC in many centres. Compared to traditional open thoracotomy, VATS offers equivalent long-term survival with reduced postoperative pain, shorter hospital stays, and faster recovery, especially when performed by an expert thoracic surgeon in London specialising in VATS and robotic lung cancer surgery.
Robotic surgery provides enhanced visualisation and precision for complex cases, including tumours near critical structures. Meta-analyses comparing robotic, VATS, and open approaches show similar five-year survival rates (approximately 73-78%), with minimally invasive techniques offering fewer complications, and many patients now consider private thoracic surgery in London using these minimally invasive approaches to reduce waiting times and optimise outcomes.
Even cases involving chest wall invasion, traditionally requiring open surgery, are increasingly managed via VATS or robotic approaches in specialist centres, with comparable survival outcomes. Post-surgery, patients undergo surveillance imaging to monitor for recurrence while recovery progresses.
Common Challenges in Managing Progression
Delayed Diagnosis Due to Lack of Symptoms
Early lung cancer rarely causes noticeable symptoms. Tumours can grow for months or years before producing persistent cough, chest pain, or other warning signs that prompt investigation. By the time symptoms appear, nearly half of lung cancer cases have reached an advanced stage, illustrating how long lung cancer can go undetected.
Solution: High-risk individuals (those over 55 with significant smoking history) should discuss lung cancer screening with their healthcare provider. If you experience symptoms, insist on prompt investigation rather than watchful waiting. Request urgent referral to a respiratory specialist for imaging tests if initial GP assessment is inconclusive.
Rapid Progression in Aggressive Types of Lung Cancer
SCLC grows so rapidly that a tumour detectable on imaging may double before the first oncology appointment if there are system delays. This leaves minimal margin for diagnostic delays or scheduling gaps.
Solution: SCLC requires expedited diagnostic workup and treatment planning, ideally within 2-4 weeks. UK data shows median time from SCLC diagnosis to systemic therapy is approximately 14-15 days, appropriate given the urgency. Patients should ensure their care team understands the aggressive nature of their diagnosis and prioritises rapid staging and treatment initiation.
Balancing Surgery Timing with Disease Progression
Surgeons must balance the time needed for proper staging, fitness optimisation, and preoperative planning against the risk that the tumour progresses during waiting periods. Too much delay may allow a resectable tumour to become unresectable. Rushing surgery without complete staging may lead to incomplete treatment, which is why understanding key insights on lung cancer surgery can be helpful for patients.
Solution: Coordinated care through a high-volume thoracic surgery centre with integrated oncology, radiology, and respiratory medicine minimises these delays. Quality improvement studies show that joint thoracic surgery-oncology clinics and patient pooling can reduce waiting times from 150 days to 110 days or less. Patients should ask their referring physician about centres with established rapid-access pathways for lung cancer diagnosis and surgery.
Conclusion and Next Steps
Lung cancer progression varies from aggressive doubling in weeks (small cell lung cancer) to slow growth over years (certain NSCLC subtypes). This variability directly influences when surgery becomes necessary and feasible. Early-stage disease (stages I-II) offers the best surgical outcomes, but delays in diagnosis and treatment erode this advantage.
Immediate actions to consider:
- Request urgent specialist referral if you have suspected lung cancer or abnormal imaging findings
- Ask about expedited staging pathways, including PET-CT and mediastinal lymph node assessment
- Discuss your case at a multidisciplinary team meeting where surgeons, oncologists, and respiratory physicians review options together
- If surgery is recommended, enquire about minimally invasive approaches (VATS or robotic surgery) and centre-specific waiting times
- If delays occur, advocate for yourself. Research shows that treatment within 40 days of diagnosis significantly improves survival
Beyond initial treatment, ongoing monitoring for recurrence and genetic testing may identify targeted therapy options if the cancer returns. The American Cancer Society and National Cancer Institute provide additional information on survival rates, treatment options, and clinical trials for advanced lung cancer.
Additional Resources
For specialist thoracic surgery consultation, patients can request a referral through their GP or directly book private thoracic surgery appointments with a consultant surgeon in London, or contact thoracic surgery centres offering private and NHS pathways. Many centres provide second opinions and rapid-access clinics for suspected lung cancer.
Lung cancer screening programmes are expanding across the UK. If you are over 55 with a significant smoking history, ask your GP about eligibility for targeted screening through local NHS initiatives or consider assessment at one of the best private hospitals in London for thoracic and lung care.
Support organisations, including Macmillan Cancer Support, Roy Castle Lung Cancer Foundation, and the British Lung Foundation, offer practical guidance for patients navigating lung cancer care. In addition, patients may benefit from resources that explain expert lung cancer surgery and recovery with minimally invasive techniques. Multidisciplinary lung cancer services can coordinate staging, treatment planning, and follow-up care to minimise delays and optimise outcomes.