Patients facing lung cancer surgery have two main options: Video-Assisted Thoracoscopic Surgery (VATS) or traditional open thoracotomy. Both are principal surgical approaches in thoracic surgery for lung cancer, with VATS representing a minimally invasive technique and open thoracotomy being the conventional method. Evidence from randomized trials and meta-analysis shows VATS delivers faster recovery, less pain, and smaller scars while achieving equivalent cancer outcomes.
This page compares VATS and open lung surgery in terms of recovery, pain, and scarring. Below is a practical comparison of both surgical approaches:
Introduction to Lung Cancer Surgery
Lung cancer surgery is a cornerstone treatment for patients diagnosed with lung cancer, especially those with early-stage lung cancer. The primary goal of lung cancer surgery is to remove the cancerous tissue while preserving as much healthy lung as possible, thereby maintaining overall lung function.
There are two main surgical approaches: Video-Assisted Thoracoscopic Surgery (VATS) and Open Thoracotomy.
For many patients, Video-Assisted Thoracoscopic Surgery has become the preferred surgical approach due to its minimally invasive nature. VATS uses small incisions and specialized instruments, resulting in fewer complications, less pain, and faster recovery compared to traditional open surgery. Randomized trials have demonstrated that VATS is an effective option for early-stage lung cancer, with a statistically significant difference in overall survival and recovery metrics when survival is compared to open surgery. VATS allows patients to benefit from advanced techniques that prioritize both cancer control and quality of life after surgery.
This guide is intended for patients and families considering lung cancer surgery, helping you understand the differences between minimally invasive VATS and traditional open surgery, and how your choice may affect your recovery, pain, and long-term results.
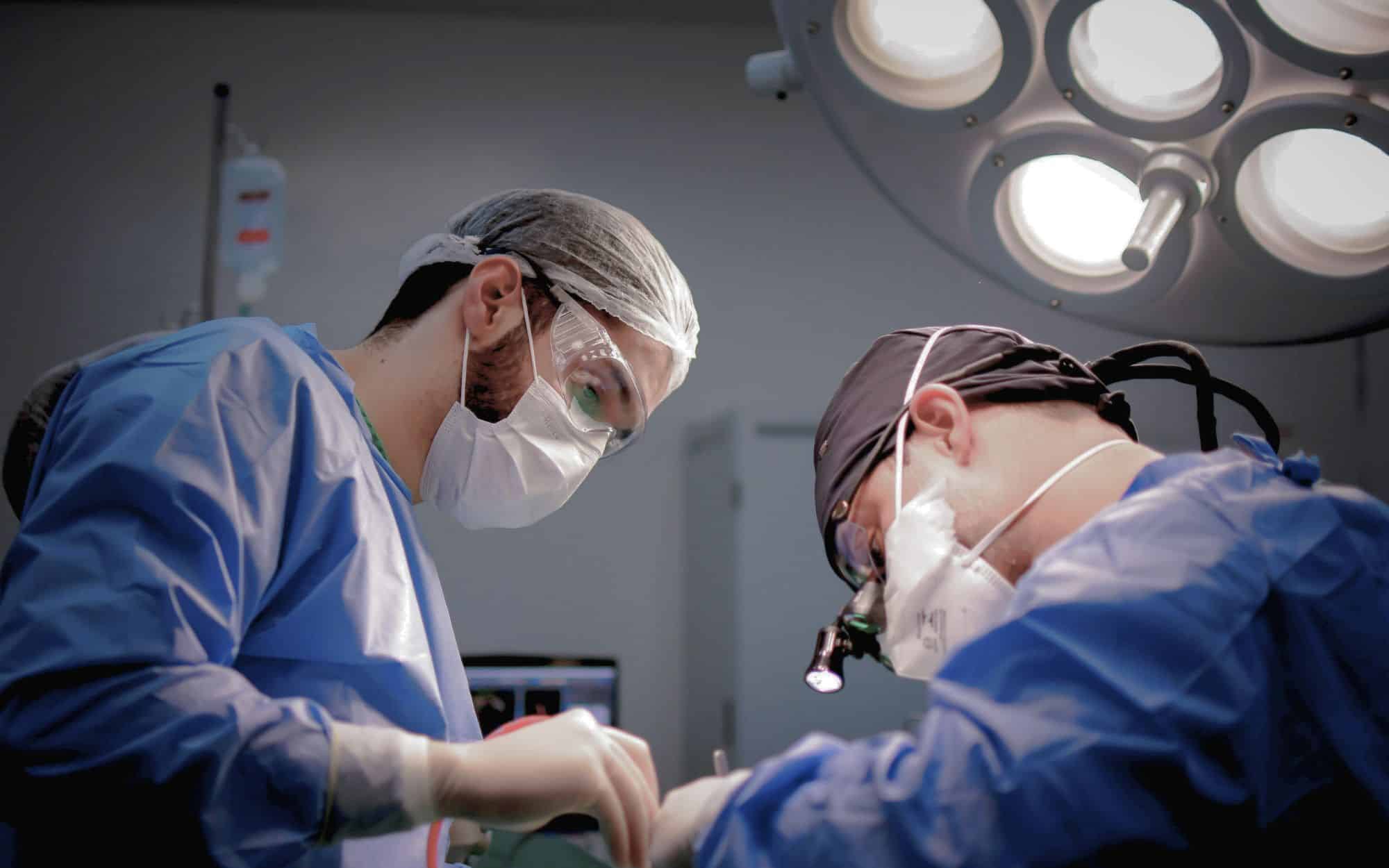
Key Differences Between VATS and Open Lung Surgery
The core distinction lies in surgical access and tissue trauma.
- Video-Assisted Thoracoscopic Surgery (VATS): VATS involves making 2–4 small incisions and using a camera and specialized instruments to access the lung. This minimally invasive technique avoids rib spreading and minimizes trauma to the chest wall.
- Open Thoracotomy (open lung surgery): This involves a larger incision (typically 10–25 cm) between the ribs, spreading or cutting the ribs, and dividing major chest wall muscles, including the latissimus dorsi and serratus. This approach allows direct access to the surgical area and is the traditional method for lung resections.
Both techniques can achieve identical surgical resection goals. Thoracic surgeons can perform lobectomy, segmentectomy, or wedge resection through either approach (learn more about the most common thoracic surgery procedures). The VIOLET (VIdeo-assisted thorascoscopic lobectomy versus conventional Open LobEcTomy for lung cancer) trial and other eligible trials demonstrate that oncological outcomes, including disease-free survival and lymph node assessment, remain comparable between methods.
However, the patient experience differs substantially. VATS offers reduced perioperative morbidity, fewer complications, and shorter hospital stays. Individual patient data from three trials shows a statistically significant difference in recovery metrics favouring minimally invasive surgery.
Comparison Table: VATS vs Open Lung Surgery
| Feature | VATS (Video-Assisted Thoracoscopic Surgery) | Open Lung Surgery (Thoracotomy) |
|---|---|---|
| Incisions | 2–4 small incisions (1–5 cm each) | Single large incision (10–25 cm) |
| Rib Spreading | No | Yes |
| Muscle Division | Minimal | Major chest wall muscles are divided |
| Hospital Stay | 3–5 days | 6–10 days |
| Recovery Time | 2–3 weeks to normal activities | 6–8 weeks to normal activities |
| Pain | Less pain, less opioid use | More pain, higher opioid use |
| Scarring | Small, less visible scars | Large, more prominent scar |
| Complications | Fewer | More |
| Cancer Outcomes | Equivalent | Equivalent |
Now that you have a general overview, let’s explore the specific differences in recovery, pain, and scarring.
Recovery Time and Hospital Stay
VATS Recovery
Hospital stays after VATS lobectomy typically range from 3–5 days in experienced centres. Some patients achieve discharge within 2–4 days when following enhanced recovery protocols.
Key recovery advantages include:
- Return to normal daily activities within 2–3 weeks
- Faster chest tube removal (often 3–5 days versus 7–12 days)
- Earlier return to work, desk jobs possible within 2-4 weeks
- Driving typically permitted within 2–3 weeks once off strong analgesia
A large US cohort study demonstrated that VATS patients had significantly shorter hospital stays compared to open thoracotomy, reflecting the quicker recovery typically seen after a keyhole lung operation. The primary analysis showed faster recovery without compromising surgical outcomes.
Open Lung Surgery Recovery
Open thoracotomy requires longer hospital stays due to greater tissue trauma. Typical admission lasts 6–10 days, sometimes extending with complications.
Recovery timeline differences include:
- 6–8 weeks before returning to normal activities
- Extended chest tube drainage requirements
- Heavy lifting is restricted for 6–8 weeks minimum
- Full chest wall strength and shoulder mobility may take 3–6 months
The follow-up period shows a gradual progression back to physical activities, with some patients experiencing residual muscle weakness or discomfort for several months.
In addition to recovery time, pain management is a key consideration for patients undergoing lung surgery.
Pain and Discomfort Levels
VATS Pain Management
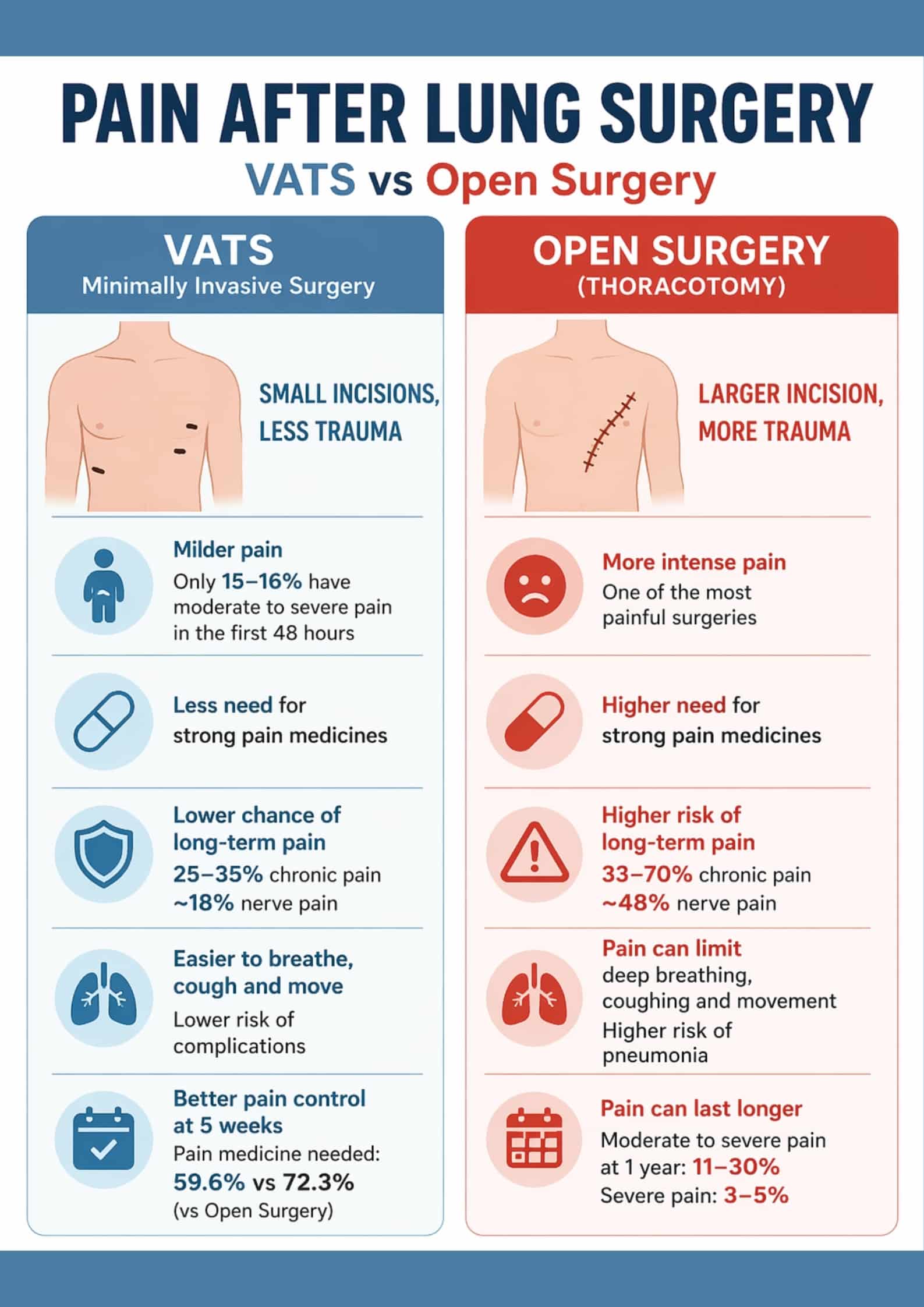
VATS produces significantly reduced pain compared to open surgery, especially when compared with the discomfort associated with the most painful thoracic incisions. Studies demonstrate that 15–16% of patients experience moderate-to-severe pain in the first 48 hours, substantially lower than thoracotomy rates.
Pain advantages include:
- A reduced need for opioid medications
- Lower rates of chronic pain development (25–35% versus 33–70%)
- Neuropathic pain in approximately 18% versus 48% for thoracotomy
- Preserved chest wall muscle function and strength
The VIOLET trial showed that postoperative pain scores at 5 weeks were lower in VATS patients. Need for analgesia after 5 weeks was 59.6% after VATS versus 72.3% after open lobectomy.
Open Surgery Pain Experience
Post-thoracotomy pain ranks among the most severe surgical pain types. Rib spreading, muscle division, and intercostal nerve trauma contribute to substantial discomfort.
Pain characteristics include:
- Higher requirements for strong opioid medications
- Potential for chronic post-thoracotomy pain syndrome in 33–70% of patients
- Significant neuropathic component from intercostal nerve damage
- Pain limiting coughing, deep breathing, and movement, increasing pneumonia risk
Long et al. and similar observational studies confirm that moderate or severe pain at one year follows thoracotomy in 11–30% of patients, with 3–5% experiencing ongoing severe pain, even though many patients are still surprised by how manageable pain and recovery can be after lung surgery.
Beyond pain, cosmetic results and scarring are also important considerations for many patients.
Scarring After VATS
VATS produces minimal visible scarring through small, strategically placed incisions.
Typical scarring involves:
- 2–4 small incisions of 1–4cm each along the chest side
- Main utility incision approximately 5cm (about 2 inches)
- Smaller scars that fade significantly over 6–12 months
- Preserved chest wall appearance and symmetry
Cosmetic outcomes prove especially important for younger patients. Better quality scarring results from avoiding major muscle division and rib manipulation.
Scarring After Open Surgery
Thoracotomy creates a single large incision with more prominent permanent scarring.
Scarring characteristics include:
- Single incision of 10–25cm along the chest or back
- Risk of hypertrophic scarring or keloid formation
- Scar maturation taking 12–18 months
- Potential chest wall contour changes from rib resection or muscle atrophy
Visible alteration to chest wall appearance may affect some patients psychologically, particularly when extensive rib work is required.
Next, let’s review how these surgical approaches compare in terms of safety and long-term outcomes.
Surgical Outcomes and Safety
VATS Surgical Results
Evidence from meta analysis demonstrates substantial survival benefits with VATS. The pooled hazard ratio shows approximately 21% reduction in mortality risk compared to open surgery.
Key outcomes include:
- Five-year overall survival of 64.9% versus 57.7% for open surgery in stage I–III disease
- Lower in-hospital mortality (0.9% versus 1.5% in matched cohorts)
- 90-day death compared: 1.8% versus 3.4%
- Fewer complications overall (23.6% versus 31.8%)
- Reduced blood loss (approximately 50–100mL versus 100–160mL)
Three studies pooling individual patient data confirm these findings with minimal statistical heterogeneity. The overall survival advantage and survival compared metrics support prioritizing VATS when technically feasible.
Sensitivity analyses controlling for baseline characteristics confirm the treatment effect is robust, with low risk of residual confounding or selection bias.
Open Surgery Results
Open thoracotomy remains the traditional gold standard with proven long term survival outcomes, particularly for complex cases.
Results underscore that open surgery offers:
- Better access for large tumours or blood vessels involvement
- Ability to handle chest wall invasion or mediastinal extension
- Proven oncological results in advanced clinical stage disease
- Flexibility for intraoperative complications
However, higher complication rates persist, including respiratory issues, longer air leak, and greater transfusion requirements, all of which form part of the broader risks for thoracic surgery. Non cancer mortality and postoperative complications remain elevated compared to VATS approaches.
Understanding the risks and complications is essential for making an informed decision about your surgical options.
Risks and Complications
All forms of lung cancer surgery carry inherent risks and potential complications. These may include bleeding, infection, and accidental injury to surrounding tissues or blood vessels. Postoperative complications such as pneumonia, respiratory failure, or prolonged air leak can also occur.
However, evidence from meta analysis and eligible trials shows that VATS is associated with a lower risk profile compared to open lobectomy, and similar benefits are seen with other minimally invasive options such as robotic-assisted lung cancer surgery. For example, pooled hazard ratio data indicate a reduced risk of death when VATS is compared to open surgery. Patients undergoing VATS typically experience fewer postoperative complications, contributing to safer recovery and improved outcomes.
It is essential for patients to discuss the specific risks and benefits of each surgical approach with their thoracic surgeon. Understanding the potential for complications and how they differ between VATS and open surgery helps patients make informed decisions about their lung cancer treatment.
The next step is to consider which patients are best suited for each surgical approach.
Patient Selection Considerations
Several factors determine the preferred surgical access for each patient:
- Tumour characteristics: VATS suits early-stage lung cancer, peripheral tumours, and smaller lesions. Large or central tumours may require open thoracotomy.
- Previous surgery: Prior chest operations creating adhesions may necessitate open approaches or risk conversion from VATS.
- Lung function: Patients with reduced pulmonary function (FEV₁ or DLCO <40%) may benefit more from VATS due to reduced perioperative morbidity, and tailored post-surgery recovery for lung cancer plans are especially important for this group.
- Overall health and age: Elderly patients often recover better from minimally invasive approaches. Higher BMI increases postoperative pain risk even with VATS, so understanding key insights on lung cancer surgery helps set realistic expectations.
- Surgeon experience: Outcomes improve significantly at high-volume centres. The Royal Brompton Hospital and similar tertiary units achieve excellent results with VATS lobectomy, supported by multidisciplinary thoracic surgery teams.
- Patient preference: Some patients prioritise faster recovery and cosmetic results; others may feel more confident with traditional open approaches.
VATS requires specialized equipment, significant surgeon expertise, and may not be suitable for large or complex tumours. The choice between VATS and open thoracotomy depends on factors such as tumour size, location, and the patient’s overall health, with VATS being preferred for smaller, accessible tumours. In advanced cases, open surgery offers the clearest view and manual control, which are essential for complex tumours. For elderly patients or those with poor pulmonary function, VATS is often preferred due to its lower physiological burden.
Bendixen et al., Lim et al., and the PLEACE trial contribute evidence supporting appropriate patient selection based on study design and eligibility criteria.
As surgical techniques continue to advance, more patients may become eligible for minimally invasive approaches.
Advances in Surgical Techniques
Recent advances in surgical techniques have transformed the landscape of lung cancer surgery. Video-Assisted Thoracoscopic Surgery (VATS) exemplifies these innovations, offering a minimally invasive alternative to traditional open surgery and forming a core part of modern thoracic surgery in London. The use of individual patient data from randomized trials has enabled more precise evaluation of the benefits and risks associated with VATS.
Technological improvements, such as enhanced imaging and refined surgical instruments, now allow thoracic surgeons to perform complex procedures with greater accuracy and safety. The VIOLET trial and other major studies have demonstrated that VATS not only improves overall survival but also reduces postoperative complications compared to open surgery. These advances ensure that patients receive the most effective and least invasive treatment possible for lung cancer.
Patient education and support are also crucial for optimal outcomes.
Patient Education and Support
Patient education and support are vital throughout the lung cancer treatment journey. Patients should be fully informed about all available surgical options, including VATS and open thoracotomy, as well as the potential benefits and risks of each approach. Understanding the importance of follow up care and regular monitoring is crucial for detecting any recurrence or spread of disease.
Thoracic surgeons play a key role in guiding patients through the decision-making process, addressing questions and concerns, and providing ongoing support. Open communication with the healthcare team helps patients feel empowered and confident in their treatment choices. Comprehensive education and support not only improve patient satisfaction but also contribute to better overall outcomes in lung cancer care.

Which Surgical Approach Should You Choose?
Choose Video-Assisted Thoracoscopic Surgery if you want faster recovery, less pain, better scars, and equivalent cancer outcomes. Evidence from the VIOLET trial and other randomized trials confirms VATS lobectomy achieves comparable disease control with reduced morbidity.
Consider open surgery if tumour size, location, or anatomical complexity makes VATS technically challenging. VATS may require conversion to thoracotomy in approximately 5-10% of cases.
For benign disease or early-stage lung cancer requiring pulmonary lobectomy, VATS represents the most common approach at experienced centres. Adjuvant chemotherapy and adjuvant treatment protocols remain identical regardless of surgical access.
Both techniques achieve excellent results when performed by experienced thoracic surgeons, whether within public systems or through private thoracic surgery in London. The two-stage approach of discussion and shared decision-making ensures patients understand the sixfold increase in certain recovery metrics favouring VATS while acknowledging situations where open lobectomy remains appropriate, a process many former patients describe positively in their thoracic surgery testimonials.
Final decisions balance tumour characteristics, patient factors, surgeon expertise, and individual preferences. The intention-to-treat basis of major trials supports either approach, achieving long-term survival goals when appropriately selected.
Which is Better: VATS or Open Lung Surgery?
Patients undergoing Video-Assisted Thoracoscopic Surgery generally report less postoperative pain, fewer complications, shorter hospital stays, and faster recovery compared to those undergoing open thoracotomy. A meta-analysis of randomized trials found that VATS lobectomy is associated with a 21% reduction in the risk of death compared to open lobectomy, without compromising disease-free survival. Both VATS and open surgery have similar long-term cancer survival rates, but VATS offers better early recovery.
VATS is the preferred approach for early-stage lung cancer and many benign conditions when technically feasible. It is currently the most common approach for pulmonary lobectomy in early-stage lung cancer, primarily due to its non-oncological benefits, such as reduced postoperative pain and faster recovery. VATS has also been shown to lead to faster physical function recovery and improved quality of life after surgery, which are significant factors in postoperative recovery.
However, open surgery remains necessary for large, complex, or centrally located tumours, and in cases where direct manual control is required. The best approach depends on tumour characteristics, patient health, and surgeon expertise. Discuss your options with your thoracic surgeon to determine the most appropriate surgical plan for your individual situation.