Slipping rib syndrome, also known as rib tip syndrome, is a condition where one or more of the lower ribs become hypermobile and slip or subluxate, causing irritation of the intercostal nerves and resulting in significant chest wall pain. The ribs specifically affected are ribs 8, 9, and 10, collectively known as the false ribs, which connect to each other via cartilage rather than directly to the sternum.
The term ‘slipping rib syndrome’ was first coined by surgeon Robert Davies-Colley in 1922.
This comprehensive guide covers the anatomy behind rib slippage, diagnostic approaches including the hooking maneuver and dynamic ultrasound, and the full spectrum of treatment options from conservative management to advanced surgical procedures such as costal cartilage excision and costal margin reconstruction. The following paragraphs are aimed at patients experiencing lower chest or upper abdominal pain, healthcare providers seeking diagnostic clarity, and individuals considering surgical consultation with a thoracic specialist. Slipping rib syndrome is often underdiagnosed and can affect both men and women of all ages, but is more common in younger individuals and athletes.
So, which ribs are affected? Slipping rib syndrome affects ribs 8, 9, and 10, the false ribs, because their unique cartilaginous attachment pattern makes them susceptible to excessive movement and displacement when the interchondral ligaments weaken or tear.
By reading this guide, you will:
- Understand precisely which ribs are affected and why floating ribs don’t slip in the same manner
- Recognise the characteristic symptoms, including intermittent sharp stabbing pain and a popping sensation
- Learn about diagnostic methods from physical examination to dynamic ultrasound
- Compare conservative, minimally invasive, and surgical treatment options with success rates
- Know when to seek specialised thoracic surgery consultation
Understanding Slipping Rib Syndrome
Slipping rib syndrome, also known as clicking rib syndrome, Cyriax syndrome, or painful rib syndrome, occurs when the cartilaginous connections between the lower ribs become unstable. This instability allows one or more ribs to move abnormally, slipping under or over adjacent ribs and compressing or irritating the intercostal nerves that run between them. The resulting pain can be severe, often mimicking cardiac, pulmonary, or gastrointestinal conditions, which contributes to frequent misdiagnosis.
The condition significantly impacts daily activities. Patients typically experience pain worse with certain movements such as twisting, reaching overhead, or deep breathing. Even simple actions like rolling over in bed or coughing can trigger episodes of sharp pain that may settle into a dull ache radiating into the upper abdomen or back.
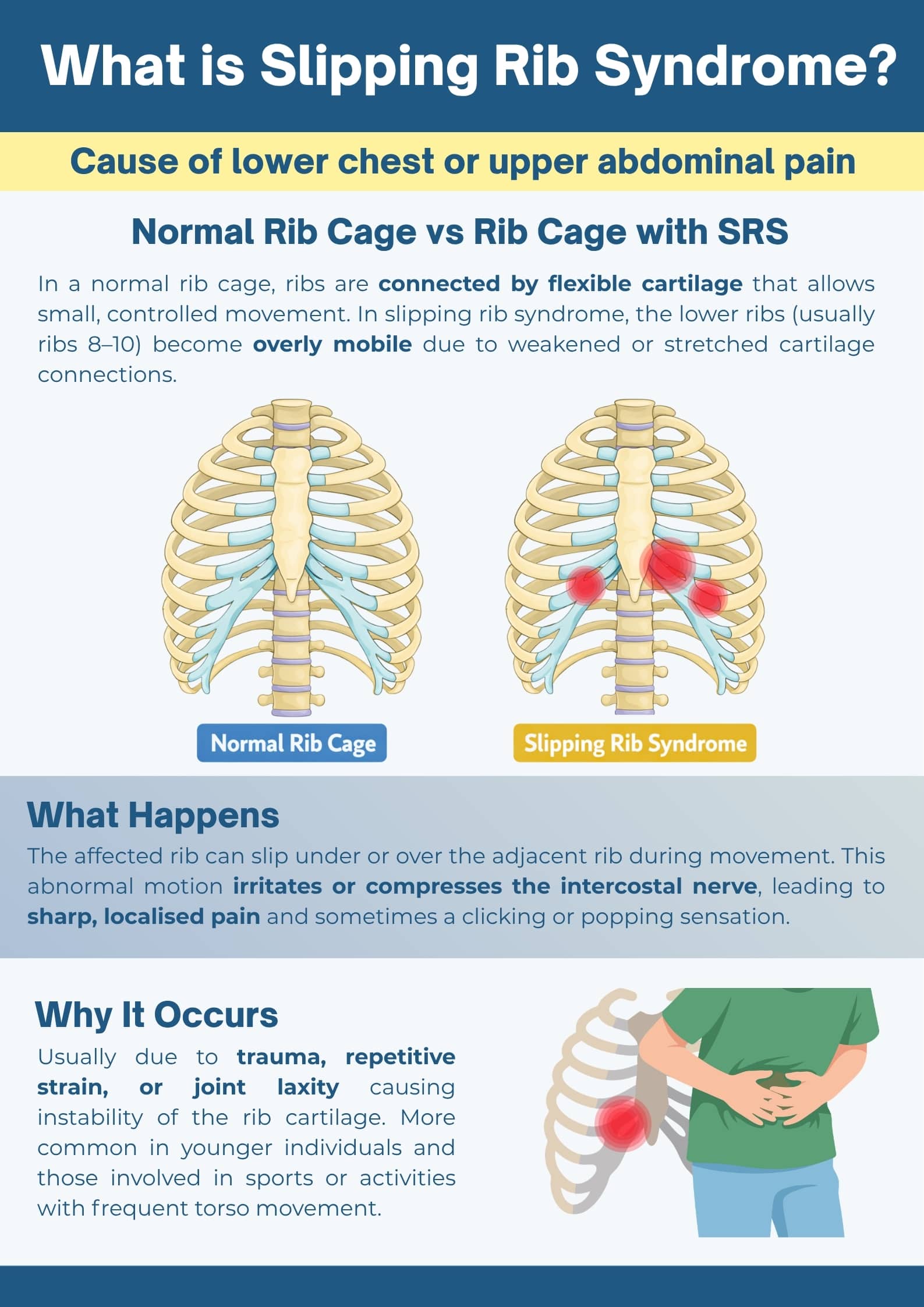
Rib Anatomy and Classification
The human rib cage comprises twelve pairs of ribs, classified into three categories based on their attachment to the sternum:
True ribs (1-7): Each connects directly to the sternum via its own costal cartilage, forming stable costosternal joints with minimal mobility.
False ribs (8-10): These do not attach directly to the sternum. Instead, they connect via cartilage to the cartilage of rib 7 and to each other through interchondral joints: fibrous and cartilaginous connections that are inherently looser than the true ribs’ attachments.
Floating ribs (11-12): Attached only to the vertebral spine posteriorly, these ribs have no anterior connection whatsoever.
The interchondral joints of the false ribs create the vulnerability central to slipping rib syndrome. When these ligamentous connections stretch, weaken, or tear due to trauma, repetitive strain, or joint laxity conditions, the affected rib gains excessive movement and can displace from its normal position. Identifying the specific rib tip affected is important for accurate diagnosis and targeted treatment of slipping rib syndrome.
Causes and Risk Factors of Slipping Rib Syndrome
Slipping rib syndrome develops when the cartilage at the interchondral joints of the lower ribs becomes weakened or displaced, allowing the rib to move abnormally. Several factors can contribute to this weakening, making certain individuals more susceptible to rib syndrome. Previous rib injury is a common cause, as trauma can stretch or tear the supporting ligaments and cartilage. Even minor injury or repetitive strain such as frequent twisting, heavy lifting, or intense coughing can gradually destabilize the rib’s attachment.
Joint laxity, whether congenital or acquired, is another significant risk factor. Individuals with naturally looser connective tissue are more prone to excessive movement of the ribs, increasing the likelihood of slipping rib syndrome. This is particularly relevant for younger patients, who may have more flexible joints and are often involved in activities that place stress on the chest wall.
Participation in sports, especially contact sports or those requiring frequent twisting motions, is also associated with a higher risk. Athletes and those engaged in sports medicine frequently present with chest wall problems, including lower rib cage pain such as rib flare and other chest wall abnormalities, which can predispose them to slipping rib syndrome. Recognizing these risk factors is essential for early diagnosis and prevention, especially in active or younger patients who may otherwise attribute their symptoms to routine muscle strain.
Symptoms and Clinical Presentation
The hallmark of slipping rib syndrome is intermittent sharp stabbing pain, typically located in the lower chest or upper abdomen. This pain often arises suddenly and may be triggered by certain movements, such as deep breathing, twisting, coughing, or sneezing. Many patients describe a distinctive popping sensation or clicking sound at the moment the rib slips, which can be both alarming and uncomfortable.
In addition to these acute episodes, a dull ache or persistent aching pain may linger in the affected area, sometimes radiating to the upper back or flank. The pain can range from mild discomfort to severe pain that interferes with daily activities. Because these symptoms overlap with other conditions, such as costochondritis (inflammation at costosternal joints of true ribs), rib flare (a postural variation), Tietze syndrome (localised swelling at the second or third costochondral junction), or even gastrointestinal issues. Differential diagnosis is crucial.
A thorough physical examination, including the hooking maneuver, is often necessary to confirm slipping rib syndrome. This test can reproduce the characteristic pain and sometimes the popping sensation, helping to distinguish rib syndrome from other causes of lower chest or upper abdominal pain. Recognizing the clinical presentation and seeking appropriate evaluation are key steps toward effective management.
Which Ribs Are Affected by Slipping Rib Syndrome
The anatomy discussed above explains why slipping rib syndrome has a highly specific anatomical distribution. Not all ribs can slip in the manner this syndrome describes. The condition is fundamentally linked to the unique structural features of particular ribs.
False Ribs (8th, 9th, and 10th Ribs)
Ribs 8, 9, and 10 are the primary and essentially exclusive sites of slipping rib syndrome. Among these, the 10th rib may be especially frequently involved due to its position at the costal margin’s most inferior and lateral aspect, where it experiences significant mechanical stress during movement.
The vulnerability stems from their attachment pattern. Rather than having individual cartilage connecting directly to the sternum, these ribs form a chain: rib 8 connects to rib 7’s cartilage, rib 9 connects to rib 8, and rib 10 connects to rib 9. This creates the costal arch, a continuous cartilaginous margin that, while allowing necessary flexibility for breathing and torso movement, lacks the inherent stability of direct sternal attachments.
Clinically, the lower rib tips affected by this syndrome produce pain in the lower chest toward the costal margin, frequently radiating to the upper abdomen or flank. This location explains why slipping rib syndrome commonly masquerades as gastrointestinal, renal, or hepatobiliary disease. Patients often undergo extensive workups for upper abdominal pain before the chest wall origin is identified.
Why Floating Ribs Don’t Slip
Ribs 11 and 12, the floating ribs, do not participate in slipping rib syndrome despite their name suggesting even greater mobility. The key difference is anatomical: floating ribs have no anterior attachment at all. They connect only to the thoracic vertebrae posteriorly and end freely in the abdominal musculature.
Because floating ribs lack interchondral joints, there is no mechanism for one rib to slip under or over another. They cannot “hook” beneath an adjacent rib because they have no cartilaginous connection to adjacent structures anteriorly.
Twelfth rib syndrome is sometimes confused with slipping rib syndrome in popular usage, but it represents a distinct condition with a different presentation, typically flank or groin pain rather than the anterior chest wall pain characteristic of true slipping rib syndrome. Accurate differential diagnosis is important because management may differ, particularly when assessing pain in floating ribs.
Unilateral vs Bilateral Involvement
The majority of slipping rib syndrome cases occur unilaterally, affecting only one side of the rib cage. Unilateral involvement typically follows direct trauma or external strain affecting one side.
However, bilateral involvement is documented and may be more common than previously recognised. One paediatric study found that approximately 23% of patients had bilateral slipping rib syndrome. Bilateral cases often follow internal stresses such as persistent coughing, repeated vomiting, or physiological changes during pregnancy, rather than external injury.
The distinction between unilateral and bilateral involvement influences treatment planning. Bilateral cases may require staged or simultaneous bilateral surgical intervention when conservative measures fail.
Diagnosis and Treatment Approaches
Accurate diagnosis of slipping rib syndrome builds directly on understanding which ribs are affected and how they move abnormally. Because the condition produces symptoms overlapping with numerous other diagnoses, a systematic approach combining clinical examination with selective investigations is essential, and patients often benefit from an essential slipping rib syndrome guide to diagnosis and treatment when learning about their condition.
Diagnostic Methods
The diagnostic pathway typically progresses through several modalities:
- Clinical examination including the hooking maneuver: The examiner places fingers under the costal margin over ribs 8-10 and lifts upward and outward. Reproduction of the patient’s characteristic pain, often accompanied by a clicking or popping sensation, constitutes a positive test. This physical examination technique remains the cornerstone of diagnosis and can be performed in any clinical setting.
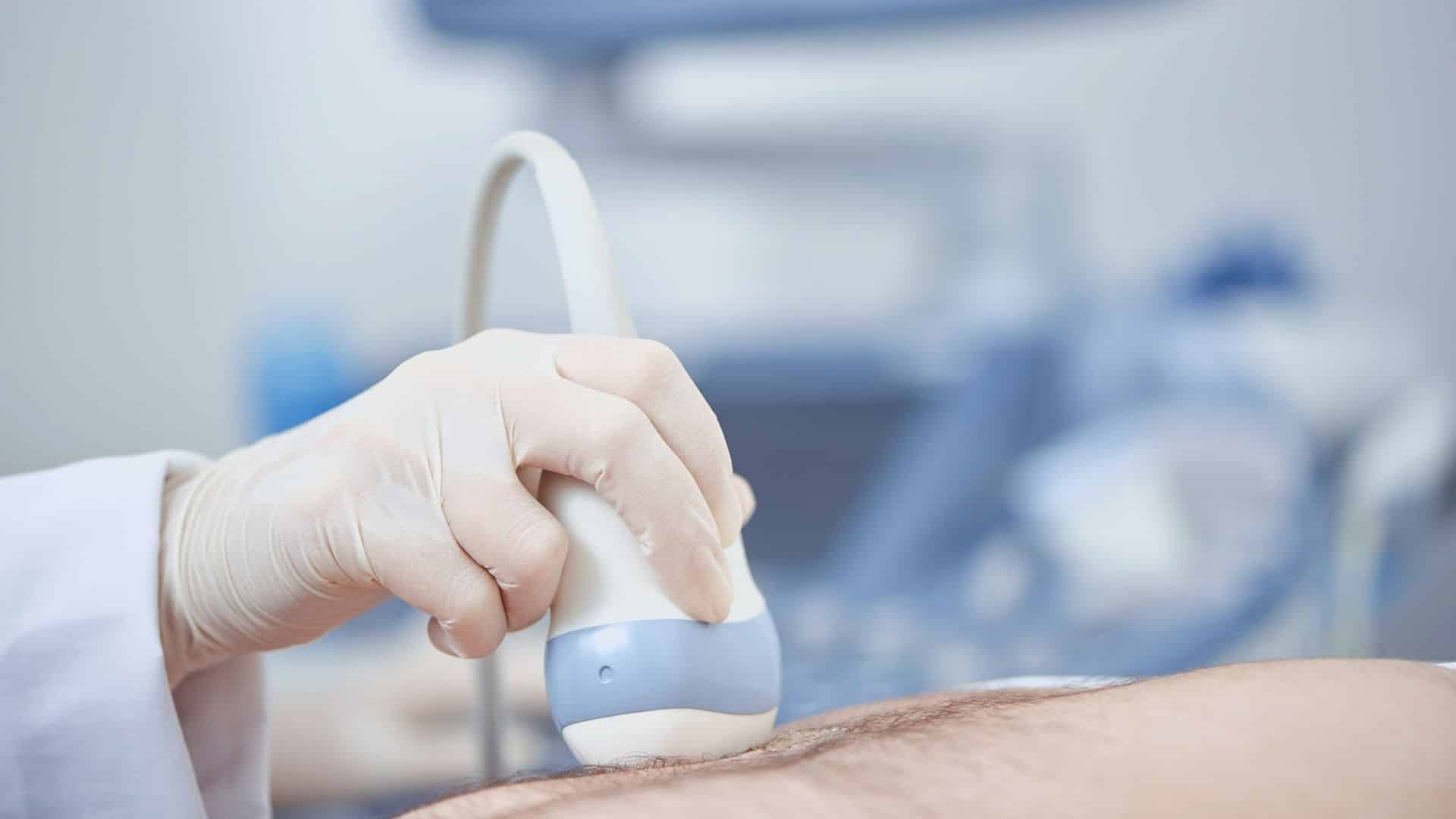
- Dynamic ultrasound assessment: Unlike static imaging, dynamic ultrasound captures rib movement in real-time as the patient coughs, twists, or performs Valsalva maneuvers. Studies demonstrate that dynamic ultrasound correctly identifies slipping rib syndrome in approximately 89% of clinically diagnosed cases, visualising abnormal cartilage mobility and rib subluxation that static imaging misses.
- Diagnostic intercostal nerve block injections: Local anaesthetic injection targeting the intercostal nerve at the affected level serves dual purposes. Pain relief following injection confirms the nerve as the pain source, while also providing temporary relief that helps patients understand what successful treatment might achieve.
- Differential diagnosis considerations: Standard imaging (X-ray, CT, MRI) rarely shows slipping rib syndrome directly, but helps exclude other conditions: rib fractures, costal cartilage pathology, thoracic disease, or abdominal conditions. When rib fractures are present, understanding potential broken ribs complications such as pneumothorax or hemothorax is vital. Screening for hypermobility disorders may be relevant, as joint laxity predisposes to rib instability.
Treatment Options Comparison
Treatment selection depends on symptom severity, duration, impact on quality of life, and response to initial interventions. The following comparison outlines the major treatment modalities:
| Approach | Description | Success Metrics | Recovery and Considerations |
|---|---|---|---|
| Conservative Management | Rest, activity modification avoiding movements that aggravate pain, NSAIDs for pain relief, hot/cold therapy, physical therapy focusing on core stabilisation. Intercostal nerve block for symptom management. | Provides pain relief for many patients; some achieve complete resolution over weeks to months. Many patients, however, have persistent or recurrent symptoms. | Low risk; gradual recovery; may take weeks to months; useful as initial approach before considering surgical procedures |
| Minimally Invasive Suture Repair | Stabilisation of the slipped rib using sutures or tape without excising cartilage. Rib-preserving approach maintaining chest wall anatomy. | Studies show approximately 75% pain improvement at one month and 80% at six months. Narcotic discontinuation in 100% by one month; NSAID cessation in 92%. | Less invasive; shorter recovery; preserves rib structure; may have higher recurrence rates requiring revision (~26% in some series) |
| Costal Cartilage Excision | Surgical removal of the affected rib tip and loose cartilage segments, partial rib resection of the displaced ribs or rib cartilage involved. | Paediatric studies show approximately 72% report complete symptom resolution; significant improvement in most others. Mean satisfaction approximately 7.8/10. | More invasive; longer recovery; 8 of 30 patients in one series required re-operation; risk of chest wall instability in children if growth centres affected |
| Costal Margin Reconstruction with Plating | Combined approach using excised cartilage as autograft spacer with bioabsorbable overlay plates to restore costal arch stability. | Lowest revision rates: approximately 1% requiring revision compared to 26% with suture-only techniques. | Most complex procedure; requires experienced thoracic surgery expertise; recovery several weeks to months; excellent long-term durability |
| The treatment progression typically moves from conservative to surgical options when symptoms persist beyond 3-6 months of conservative management or when pain significantly impacts daily function. |
Physical Therapy and Rehabilitation
Physical therapy is a cornerstone of conservative management for slipping rib syndrome, aiming to provide pain relief, restore function, and prevent recurrence. A tailored rehabilitation program focuses on strengthening the muscles that support the affected rib and improving overall chest wall stability. Treatment modalities may include targeted exercises to enhance posture, core strength, and breathing mechanics, as well as manual therapy techniques to reduce pain and inflammation around the affected rib.
In some cases, intercostal nerve blocks may be used to provide temporary relief, allowing patients to participate more fully in physical therapy. Collaboration with a pain physician or a physical therapist experienced in sports medicine and thoracic disease ensures that the rehabilitation plan addresses the unique needs of each patient. By combining exercise, manual therapy, and pain management strategies, physical therapy can help many individuals with slipping rib syndrome regain mobility and reduce symptoms without the need for surgery, especially when integrated with an essential slipping rib syndrome resource on diagnosis and treatment.
Intercostal Nerve Involvement
A key feature of slipping rib syndrome is the involvement of the intercostal nerves, which run along the underside of each rib and are responsible for transmitting pain signals from the chest wall to the brain. When a rib slips or subluxates, it can irritate or compress these nerves, resulting in severe pain that is often sharp and localized.
To both diagnose and manage this nerve-related pain, intercostal nerve blocks are frequently employed. These injections deliver local anesthetic to the affected nerve, providing temporary relief and confirming the source of the pain. For patients who do not achieve lasting improvement with conservative measures, surgical procedures such as costal cartilage excision or partial rib resection may be necessary, and in other chest conditions, patients may even require pneumothorax surgery. These interventions aim to remove or stabilize the segment of rib or cartilage causing nerve compression, offering more definitive relief from the symptoms of rib syndrome.
Common Challenges and Solutions
Despite being well-documented in medical literature including the British Medical Journal and Paediatric Respiratory Reviews, slipping rib syndrome presents several recurring challenges in clinical practice.
Delayed or Misdiagnosis
Slipping rib syndrome accounts for approximately 1% of diagnoses in general medical clinics, but rises to 5% in gastroenterology settings evaluating chest or upper abdominal pain. This disparity highlights how frequently the condition is initially attributed to gastrointestinal, cardiac, or pulmonary causes.
Solution: The condition tends to affect younger patients; paediatric series show median symptom onset around age 14, and demonstrate female predominance (approximately 86% in some cohorts). Awareness of these demographics, combined with routine use of the hooking maneuver when evaluating lower chest wall pain, improves detection. Early referral to a thoracic surgeon experienced with chest wall problems prevents prolonged diagnostic delays.
Inadequate Conservative Treatment Response
Many patients with confirmed slipping rib syndrome do not achieve adequate pain management through conservative measures alone. Rest and physical therapy may provide temporary relief without addressing the underlying mechanical instability.
Solution: A progressive treatment approach proves most effective. Initial conservative management establishes baseline response. Intercostal nerve block with local anaesthetic and corticosteroid can provide temporary relief lasting weeks to months while helping confirm the diagnosis. When conservative measures fail to provide sustained benefit after 3-6 months, surgical intervention becomes appropriate. This stepwise approach avoids both premature surgery and unnecessarily prolonged suffering.
Surgical Decision-Making
Determining surgical candidacy and selecting the optimal technique present challenges. Earlier surgical approaches showed variable outcomes: suture-only repair required revision in approximately 26% of patients, while costal cartilage excision alone sometimes led to recurrence or, in children, chest wall growth disturbance.
Solution: Comprehensive evaluation by an experienced thoracic surgeon allows individualised surgical planning. Modern techniques including costal margin reconstruction with bioabsorbable plating demonstrate revision rates as low as 1%. For paediatric surgery cases, rib-preserving techniques that avoid growth centre disruption offer advantages. The anterior cartilaginous part of the rib, while structurally important, can be addressed through reconstruction rather than simple excision when expertise permits.
Complications and Prognosis
If slipping rib syndrome is not properly treated, it can lead to ongoing complications such as chronic pain, restricted movement, and a reduced quality of life. In rare instances, persistent chest wall pain may contribute to secondary issues, including respiratory difficulties or, very infrequently, cardiac concerns due to altered breathing patterns or anxiety.
The prognosis for slipping rib syndrome is generally favorable, especially when patients receive timely and appropriate care. Most individuals experience significant improvement with a combination of pain management, physical therapy, and, when necessary, surgical intervention. However, some patients may have persistent or recurrent symptoms, requiring ongoing support and symptom management.
A multidisciplinary approach incorporating the expertise of pain physicians, physical therapists, and thoracic surgeons who manage a wide range of thoracic conditions can optimize outcomes and help patients return to normal activities. Regular follow-up is important to monitor progress, address any complications, and adjust treatment as needed, ensuring the best possible prognosis for those affected by rib syndrome.
Conclusion and Next Steps
Slipping rib syndrome specifically affects ribs 8, 9, and 10 (the false ribs) due to their unique interchondral joint attachments that create vulnerability to hypermobility and subluxation. The floating ribs (11 and 12) do not slip in this manner because they lack anterior cartilaginous connections. Treatment ranges from conservative pain management through minimally invasive stabilisation to definitive surgical reconstruction, with modern techniques achieving excellent outcomes and low revision rates.
Immediate steps for patients experiencing symptoms:
- Document your pain patterns: location, triggers, duration, and any slipping sensation or popping sounds.
- Request the hooking maneuver during your next clinical appointment if slipping rib syndrome hasn’t been considered.
- If initial imaging and gastrointestinal workup proves unrevealing, request referral to a thoracic surgeon experienced in chest wall conditions.
- Bring this documentation to your consultation to facilitate efficient evaluation.
Additional Resources
For patients seeking specialist evaluation for slipping rib syndrome or other chest wall problems, Mr. Marco Scarci offers both virtual consultations and in-person assessments. Virtual consultations allow initial case review, imaging interpretation, and guided self-examination techniques prior to clinic attendance.
In-person consultations include a comprehensive physical examination with the hooking maneuver and, where indicated, a dynamic ultrasound assessment to demonstrate excessive movement of the affected area. For patients with confirmed diagnosis requiring surgical intervention, Mr. Scarci performs advanced thoracic surgery techniques including minimally invasive stabilisation and costal margin reconstruction.
To arrange a consultation for slipping rib syndrome or related chest wall conditions, contact Mr. Marco Scarci’s practice directly for appointment availability and referral requirements or visit his consultant thoracic surgeon London appointments page.