Chest wall pain originating from the musculoskeletal structures of your chest: ribs, cartilage, muscles, and sternum, affects many patients who struggle to determine whether their symptoms require specialist evaluation. Musculoskeletal causes are the most common source of chest wall pain, often resulting from issues such as a pulled muscle, costochondritis, or rib injuries.
However, when chest pain persists beyond 4-6 weeks despite conservative treatment, or presents with concerning features such as a palpable mass or unexplained weight loss, consultation with a thoracic surgeon becomes necessary to rule out serious underlying conditions, including rare associations with previous breast cancer treatment such as surgery or radiotherapy, and to explore appropriate treatment options. It is also important to consider other symptoms, such as night pain, fatigue, or systemic signs, which may indicate systemic or non-musculoskeletal origins.
This guide covers persistent musculoskeletal chest wall pain requiring specialist assessment and explains what distinguishes it from emergency situations. Life-threatening causes such as heart attack, pulmonary embolism, aortic dissection, or tension pneumothorax require immediate emergency evaluation and fall outside the scope of this article. These conditions demand urgent medical attention rather than planned specialist referral.
It is for patients experiencing ongoing anterior chest wall pain lasting more than 4-6 weeks, those with concerning features like a growing mass or severe pain unresponsive to treatment, and healthcare professionals seeking guidance on appropriate referral pathways to thoracic surgery.
Red flag symptoms warranting prompt medical attention include: a firm, growing chest wall mass (particularly if fixed or painful); chest pain with systemic symptoms such as unexplained weight loss or night sweats; pain unrelieved by rest that worsens with deep breathing; chest wall deformity or instability following direct trauma; and imaging findings showing bone destruction or suspicious masses. It’s recommended that people experiencing these symptoms consult with specialists like Mr Marco Scarci in London for a proper assessment.
Understanding Chest Wall Pain

Chest wall pain refers to discomfort arising from the musculoskeletal structures of your chest, with musculoskeletal causes being the most common source. These include conditions such as costochondritis, rib injuries, and soft tissue strains (a pulled muscle is a frequent example). Unlike cardiac chest pain, which often radiates to your upper arm or jaw and accompanies exertion, musculoskeletal chest pain typically localises to specific areas and worsens with certain movements, breathing deeply, or direct pressure on the painful area.
The chest wall comprises multiple anatomical structures that can generate pain: the rib cage with its bony framework, cartilaginous connections coupled to the sternum at the costochondral joints, intercostal muscles supporting respiration between ribs, the costovertebral joints where ribs join the thoracic spine, and the soft tissues, including fascia and neurovascular bundles running along each rib. Chest wall pain can feel like a pulled muscle, may be burning or sharp, can be localized to one side or spread across a wider area, and is sometimes accompanied by a deep itching sensation that is not relieved by scratching.
Acute vs Persistent Chest Wall Pain
Acute chest wall pain typically results from recent injury. These can be muscle strains from heavy lifting, rib contusions from direct trauma, or inflammation at the costosternal syndrome sites following severe coughing. Most commonly, musculoskeletal conditions of this nature resolve within a few weeks with conservative care, including rest, anti-inflammatory medications, and heat packs, alongside structured strategies for fractured rib pain management and recovery.
Persistent chest wall pain, defined as symptoms lasting beyond 4-6 weeks despite adequate treatment, represents a different clinical picture requiring closer evaluation. This chronicity may indicate non-union of fractures, stress fracture, underlying swelling of joints, or more serious pathology such as tumour development. The distinction matters significantly: acute pain usually requires patience and supportive care, whilst persistent pain demands investigation to identify any underlying cause requiring specialist intervention.
Common vs Concerning Features
Typical musculoskeletal chest wall pain presents with several reassuring characteristics: localised tenderness reproducible by pressing the painful area, pain increases with arm overhead movements or lateral flexion, discomfort worsening when breathing deeply or lying on the affected side, and improvement with rest and standard analgesia. Pain may be constant or intermittent and can be accompanied by other sensations such as numbness or tingling. This pattern suggests conditions like costochondritis, muscle strains, or inflammatory conditions affecting the costochondral joints, which are generally self-limiting conditions responding to conservative management.
Concerning features that suggest more serious underlying pathology include the following:
- a palpable mass that is firm, growing, or fixed to underlying structures
- sharp chest pain unrelieved by rest or standard painkillers
- anterior chest pain accompanied by unexplained weight loss, night sweats, or feeling sick
- neurological symptoms such as numbness or burning sensation suggesting nerve involvement; respiratory compromise, including progressive breathlessness
- and pain that persists despite several weeks of appropriate treatment
It is also important to identify other symptoms such as night pain, fatigue, or systemic signs that may suggest systemic, rheumatic, or non-musculoskeletal causes of chest pain and support a comprehensive assessment. These red flags warrant specialist evaluation rather than continued GP management, as they may indicate tumours, complex nature injuries, or other conditions requiring surgical expertise.
Types of Chest Wall Conditions Requiring Specialist Care
Building upon the distinction between common chest wall symptoms and concerning presentations, certain conditions specifically require thoracic surgery evaluation due to their complexity and potential need for surgical intervention. Understanding these categories helps patients and referring clinicians recognise when specialist input becomes essential.
Chest Wall Tumours and Masses
Chest wall tumours account for fewer than 5% of thoracic neoplasms, encompassing both primary growths arising from bone or soft tissues and secondary tumours invading from adjacent structures such as lung cancer infiltration. Primary tumours include benign conditions like osteochondroma and fibrous dysplasia, as well as malignant types, including chondrosarcoma, osteosarcoma, and Ewing sarcoma within the broader group of thoracic sarcomas and chest wall tumours.
Patients typically present with a visible or palpable mass, localised sharp pain worsening with movement or inspiration, and sometimes breast pain when tumours affect anterior structures. Breast pain is usually not linked to breast cancer, but it can sometimes be associated with previous breast cancer treatment such as surgery or radiotherapy. Pain caused by other medical conditions, such as angina or gallstones, may also present as breast pain and require medical evaluation for proper diagnosis and treatment.
Clinical examination often reveals a hard mass attached to bone or cartilage, potentially accompanied by localised swelling. UK surgical data demonstrates that approximately half of operated chest wall tumours involve lung cancer with chest wall infiltration, with the remainder representing primary tumours, emphasising the importance of expert evaluation for any suspicious mass.
Chest Wall Deformities
Pectus excavatum, where the sternum appears concave or sunken, occurs in approximately 1 in 400 births and represents the most common chest wall deformity, with male predominance of roughly 4:1.
Pectus carinatum, featuring a protruding chest wall, affects about 1 in 1,500 individuals.
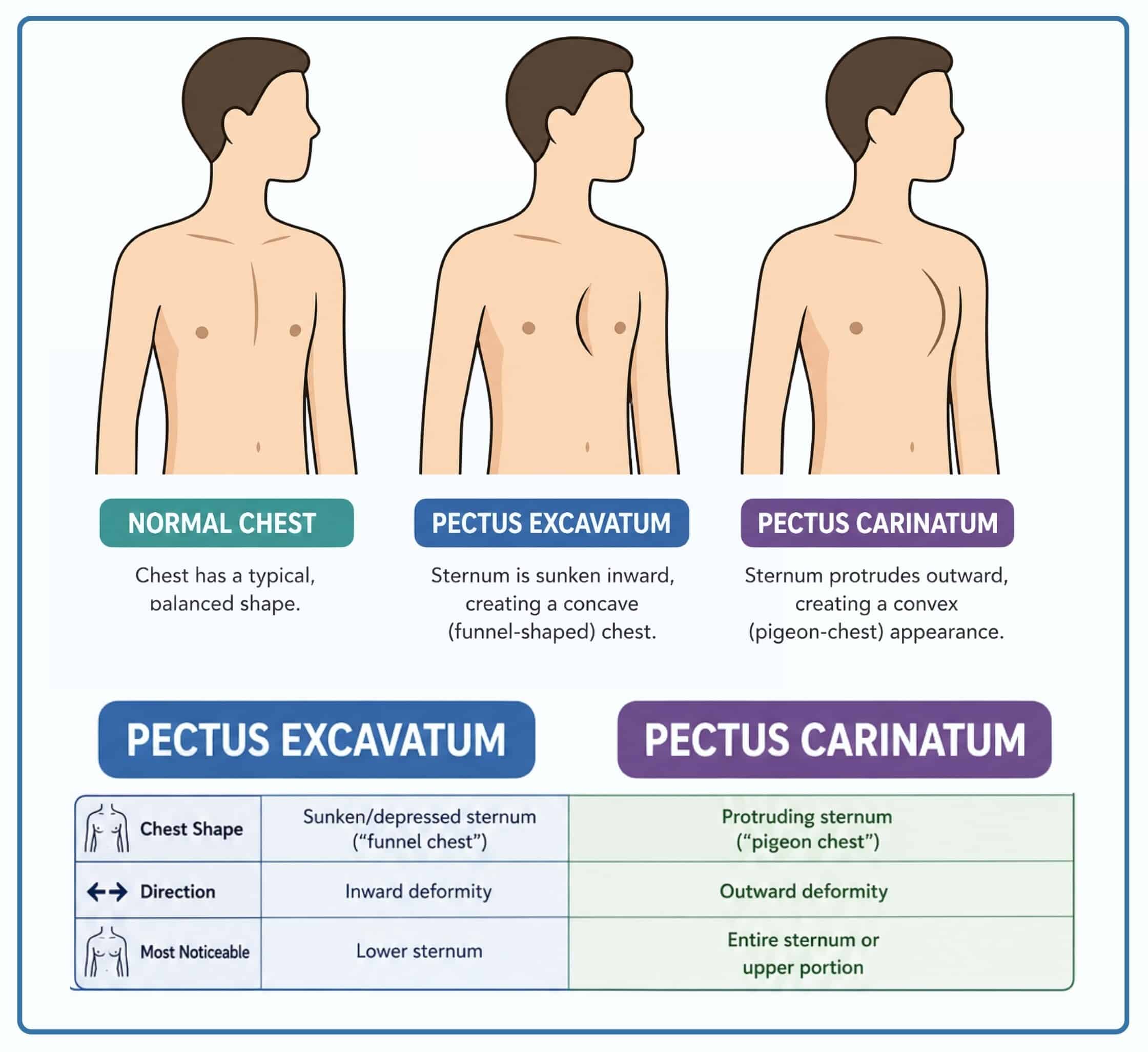
Beyond aesthetic concerns, these deformities can cause anterior chest wall pain, back pain affecting the thoracic spine, breathlessness particularly with exertion, and palpitations due to cardiac compression.
Assessment involves CT imaging to calculate the Haller index (values exceeding 3.2 indicating pathology), lung function tests, and echocardiography. Treatment options range from non-surgical approaches like vacuum bell therapy and bracing to minimally invasive surgical techniques such as the Nuss procedure for excavatum correction.
NHS England policy currently restricts routine surgery but permits individual funding requests where functional impairment is demonstrated.
Rib Fractures and Trauma Complications
While most isolated rib fractures heal spontaneously with conservative care over a few weeks, understanding the potential long-term effects of broken ribs is important, and certain fracture patterns require surgical expertise. Complex injuries warranting specialist evaluation include: flail chest and other serious broken rib complications where a segment of chest wall becomes detached and moves paradoxically with breathing; three or more severely displaced fractures with bicortical displacement; pathological fracture through diseased bone; open fractures or pulmonary herniation; and persistent severe pain despite adequate analgesia. Non-union or malunion following initial conservative management also requires surgical assessment.
In these cases, a biomechanical assessment is often valuable to evaluate rib fractures and musculoskeletal injuries, particularly for broken rib injuries from winter accidents, reviewing training loads, physical function, and movement patterns, frequently in conjunction with physiotherapy interventions, to inform management and help prevent future injury. Modern surgical rib fixation using plates and screws, often performed through minimally invasive approaches, including thoracoscopy, has demonstrated reduced hospital stays, less ventilator dependence, improved pain control, and faster functional recovery compared to prolonged conservative management in appropriate cases.
Key points from this section: Chest wall tumours require biopsy and potential wide excision with reconstruction; deformities need objective assessment and may qualify for surgical correction when functional impairment exists; complex rib trauma benefits from early surgical stabilisation in selected patients rather than prolonged conservative management.
Specialist Evaluation Criteria and Process

Having established which chest wall conditions may require surgical expertise, it’s important to note that musculoskeletal causes are common, often self-limiting, and require specific assessment and management strategies, which distinguishes them from systemic or life-threatening conditions. Understanding the specific criteria that differentiate GP-manageable symptoms from those requiring specialist referral helps patients and clinicians make appropriate decisions about care pathways.
Red Flag Symptoms for Immediate Referral
The following features should prompt timely referral to a thoracic surgeon rather than continued GP observation:
- A firm, growing chest wall mass, particularly if fixed to underlying structures, painful on palpation, or hard in consistency
- Chest wall pain accompanied by systemic symptoms, including unexplained weight loss, night sweats, or constitutional features suggesting malignancy
- Pain unrelieved by rest with neuropathic characteristics (numbness, trigger points, burning sensation) suggesting involvement of intercostal nerves
- Chest wall deformity emerging or progressing, or visible instability with paradoxical movement following trauma
- Persistent pain beyond 4-6 weeks despite adequate conservative therapy including physiotherapy, particularly post-trauma fractures showing evidence of non-union or malunion
- Imaging findings demonstrating chest wall infiltration, bone destruction, or suspicious mass on CT or MRI
Specialist vs GP Management Comparison
| Criterion | GP Management Appropriate | Specialist Referral Needed |
|---|---|---|
| Duration | Pain less than 4-6 weeks; symptoms improving with rest and treatment | Symptoms persist beyond 4-6 weeks without improvement; worsening despite treatment |
| Pain characteristics | Mild to moderate isolated musculoskeletal chest pain; reproducible by movement; responds to NSAIDs and physiotherapy | Severe pain; constant or progressively worsening; pain bilaterally or at rest/night; neuropathic features; non-responsive to multimodal analgesia |
| Associated symptoms | No systemic features; local bruising or underlying swelling only; normal breathing and heart rate | Systemic signs (weight loss, fevers); respiratory symptoms; visible deformity; palpable mass; neurological deficits affecting chest or upper arm |
| Imaging findings | Normal or minor musculoskeletal changes; simple rib fracture without significant displacement; no suspicious mass | CT/MRI showing mass or tumour; multiple displaced rib fractures; chest wall instability; bone destruction or infiltration of adjacent structures |
| This comparison helps patients understand that most chest wall symptoms appropriately receive initial GP management with strengthening exercises, local anaesthetic injections for costochondritis, and monitoring. Specialist referral becomes necessary when symptoms persist, worsen, or develop concerning features—not as a reflection of failure but as appropriate escalation to access diagnostic capabilities including biopsy and advanced imaging interpretation, plus surgical interventions when indicated. |
Common Concerns About Specialist Referral
Patients frequently experience hesitation about specialist referral, whether due to worry about serious diagnoses, uncertainty about timing, or questions about what treatment might involve. Addressing these concerns directly supports informed decision-making.
Worry About Serious Diagnosis
Concern about cancer or other serious conditions is understandable, but should not delay necessary evaluation. Early specialist assessment improves outcomes when serious pathology exists. For chest wall sarcomas, achieving clear surgical margins at resection significantly influences recurrence risk and survival. Importantly, many chest wall masses prove benign, and specialist evaluation provides definitive answers through imaging and biopsy rather than prolonged uncertainty.
Whether the diagnosis reveals a concerning condition requiring treatment or provides reassurance that conservative management remains appropriate, early clarity benefits patients psychologically and clinically.
Uncertainty About Referral Timing
The practical guidance follows the “4-6 week rule”: if your chest wall pain persists beyond four to six weeks of appropriate conservative management, or if symptoms worsen rather than improve, specialist referral should be considered. Any symptoms persist alongside red flag features such as mass development, systemic symptoms, and chest wall instability all warrant earlier referral regardless of duration. Monitor your symptom trajectory: improving symptoms supports continued conservative care, whilst stable or worsening pain despite treatment indicates referral benefit. For trauma patients with severe displacement, respiratory compromise, or a chest that feels tight with paradoxical movement, earlier surgical consultation (within days rather than weeks) may be appropriate.
Questions About Treatment Options
Modern thoracic surgery offers significantly less invasive approaches than historical procedures. Rib fracture stabilisation now utilises smaller incisions, often with thoracoscopic assistance, reducing soft tissue trauma and enabling faster recovery.
Techniques like intercostal nerve cryoablation provide enhanced pain control. For pectus deformities, minimally invasive bar techniques have largely replaced extensive open surgery, though both remain available depending on individual circumstances.
Tumour resection may require reconstruction using mesh, titanium plates, or muscle flaps, with treatment plans individualised based on tumour characteristics and patient factors.
Understanding that modern surgical options exist (less invasive than many patients imagine) helps alleviate concerns about referral while ensuring appropriate conditions receive timely expert evaluation.
Conclusion and Next Steps
Recognising when persistent chest wall pain requires specialist thoracic surgery evaluation empowers patients to seek appropriate care at the right time. Most musculoskeletal chest pain responds to conservative management, but symptoms lasting beyond 4-6 weeks, concerning features such as masses or systemic symptoms, and complex trauma patterns warrant specialist assessment to access advanced diagnostic capabilities and surgical treatment options when needed.
For patients experiencing persistent chest wall symptoms:
- Document your symptom timeline: When the pain started, what treatments you have tried, and whether symptoms are improving, stable, or worsening
- Note any red flag features, including masses, weight loss, night pain, or respiratory symptoms
- Discuss referral with your GP if symptoms persist beyond 4-6 weeks or concerning features develop
- Request imaging results (CT or MRI reports) to bring to specialist consultations
- Prepare questions about diagnosis, treatment options, and expected outcomes for your specialist appointment
Related conditions that may require similar evaluation include chest infections (such as pneumonia), which can cause chest wall pain or discomfort and should be distinguished from heart-related causes. Other differential diagnoses include isolated chest wall infections not responding to antibiotics, post-surgical chronic pain problems following previous thoracic procedures, and anterior chest pain with underlying swelling suggestive of inflammatory conditions affecting multiple joints or ankylosing spondylitis affecting the costovertebral joints.
Costochondritis (also known as costosternal syndrome) is the most common specific cause of anterior musculoskeletal chest pain, with a prevalence of 13%. Tietze syndrome is similar to costochondritis but is characterized by visible swelling. Lower rib pain syndrome presents with pain in the lower chest or upper abdomen and is thought to result from inadequacy or rupture of the interchondral fibrous attachments of the anterior ribs, allowing subluxation of the costal cartilage tips. Slipping rib syndrome occurs when the ligaments of the lower ribs move, causing sharp discomfort.
The sternalis muscle, including the overlying sternalis muscle, is a potentially under-recognized source of anterior chest wall pain and localized tenderness. Sternalis syndrome, which may be more common than previously thought, presents as anterior chest pain characterized by localized tenderness over the sternum or sternalis muscle, with palpation often provoking radiation of pain on both sides. This condition is considered relatively common in general practice, is believed to be self-limiting, and is unlikely to cause persistent pain.
Things To Keep In Mind When Consulting A Specialist
Preparing for consultation: Bring a summary of your symptom history, previous imaging on disc or via image-sharing platforms, a list of current medications, and specific questions about your condition. Having a clear understanding of symptom duration and progression makes it easier to assess your situation.
Appointment information: Thoracic surgery consultations are available both through NHS referral pathways and private services. Waiting times vary; patients with red flag symptoms may access urgent pathways through their GP.
Emergency protocols: Sudden chest pain accompanied by breathlessness, sweating, pain radiating to the jaw or upper arm, or a blood clot in your legs with sudden breathlessness requires immediate emergency department attendance rather than planned referral. These potentially life-threatening causes require urgent assessment regardless of any existing chest wall condition.